Health
Ugandan Legislators applaud MakSPH for Road Safety & Injuries Research
Published
4 years agoon

Members of Parliament under the Parliamentary Forum on Road Safety (PAFROS) have commended research efforts by the Makerere University School of Public Health’s Trauma and Disability Unit (TRIAD) for its leadership in injury and prevention research. The legislators signed a commitment to support all efforts aimed at improving road safety in Uganda.
The legislators said this while at an engagement meeting with researchers at MakSPH that took place on Thursday 17th February 2022 at Sheraton Hotel. In a well-attended session, the research team shared evidence from a number of publications that have influenced policy, and over 10-11 years, and the several achievements the School has achieved in collaboration with partners both national and international.

The 2014 WHO Global Health Estimates show high burden of injuries with over five million people dying of injuries every year. Mr. Frederick Oporia, a PhD fellow says nearly every six seconds, someone dies from an injury leaving over 50 million people with disabilities.
Despite this, there is insufficient research capacity to drive prevention and management of these injuries which makes multidisciplinary approach in handling multidisciplinary nature of injuries.

TRIAD’s main objective is to contribute to the reduction of injury burden in Uganda by strengthening research capacity on injuries and their medical, social and economic consequences both at Individual, community and National level.
There are various kinds of injuries that range from being intentional and non-intentional. Some of these include violence, burns, poisoning, drowning, falls and road traffic crashes. In all these injuries, road traffic contributes the highest burden 24% hence a big problem.
Currently, TRIAD focuses on mobility, Road Traffic Injury prevention, drowning prevention, childhood injury prevention and emergency Trauma Care and emergency medical services.
“When we compare HIV, tuberculosis and Malaria rates, we see that injuries alone almost double what these other Disease claim and it’s a problem we need to tackle,” says Oporia.
Goal 3 of the Sustainable Development Goals (SDGs) seeks to ensure health and well-being for all, at every stage of life. Equally so, the UN Decade of Action included road safety in the framework of Sustainable Development Goals with an ambition to halve road traffic deaths and injuries by 2020.
The 2011-2020 decade of action for road safety was premised on five pillars that included road safety management, safer roads and mobility, safer vehicles, safer road users, and post-crash response.
However, trends analysis in the Uganda Police Reports show that Uganda instead increased road traffic crashes. The SDG Goal 11 that commits UN member States to make cities and human settlements inclusive, safe, resilient and sustainable ambitiously states that by 2030, the member states should be able to provide access to safe, affordable, accessible and sustainable transport systems for all, improving road safety, notably by expanding public transport, with special attention to the needs of those in vulnerable situations, women, children, persons with disabilities and older persons.

The Road safety performance review report of 2018 show that Uganda’s road safety management is managed in the Ministry of Works and Transport under the Directorate of Road Transport. Some of the road transport legislations include, the Traffic and Road Safety Act (Amended) 2020, the Uganda National Roads Authority Act, 2006, the Uganda Road Fund Act, 2008, the National Road Safety Policy, 2014 and the Non-Motorized Transport policy, 2012.

Speaking to the legislators, Esther Bayiga Zziwa, a PhD fellow at MakSPH’s TRIAD unit says however that Uganda has legislative gaps in majority of the risk factors for instance, while Uganda has national drink-driving law in place, and drink – driving based on Blood Alcohol Content (BAC) or equivalent breath alcohol concentration (BrAC), the BAC limit for the general population is way higher than the global standard. The global standard is at below 5 gram per blood liter. However, in Uganda, the law puts it at 7 gram per blood liter which is high. Ms. Bayiga says there is a need to handle this back to the global level.
Uganda has a national motorcycle helmet law in place which applies to motorcycle drivers and adult passengers and to all road types an engine type. However, the law does not require helmets to be properly fastened as well as meet the national and or international standards.
“Helmets standards for motorcyclists put up by Uganda National Bureau of Standards (UNBS) need to make sure that those ones on market meet the standards and if you are found wearing a fake helmet, you are not better off than one not wearing any because in case of a crash, it will damage your head instead of protecting it, and people need to fasten their Helmets for better effectiveness,” says Bayiga.
Research on road safety has found that behaviour interventions area not as effective as environmental, legislative and enforcement actions. Bayiga says the Behavioural component alone cannot be effective. She recommends a multipronged approach that includes bbehavioural, environmental modification, enforcement and legislation in road safety regulation.
Uganda lacks a national child restraint law based on age, weight, height or a combination of these factors that would restrict children under a certain age-height from sitting in the front seat.
“In Uganda, even here in Kampala, those who can afford cars do not buy child safety seats for their babies and the children are carried by other adults and do not have a seat on their own. However, in case of a clash, those are the first ones that fall off the car because of their body mass and can’t survive with the normal seat,” Bayiga says.

According to Bayiga, other countries have the regulations but; “Our law does not take account any with regarding children, and probably some people think cannot afford, but this can not be compared to the lives and value of children, they too need safe seat because every life matters and a law should be put in place to address this.”
Hon. Linda Irene Mugisa, the Fort portal City Woman MP and member of the Road Safety Forum acknowledges the role of legislators to make laws and policies that would protect Ugandans.

“We have a big role of sensitizing the masses. Right now, we have very many youths who are earning income through riding boda-bodas. And the unfortunate part of this is that most of these youths have not gone through training and most of them are riding illegally because some cannot afford the driving permits. As members of parliament we feel we should advocate for the reduction in the amount of money a rider requires in order to acquire a driving permit,” says Hon. Linda.
Juliet Bashiisha Agasha, the Woman MP for Mitooma District said she was impressed by the dialogue and was excited to learn that indeed, the Trauma, Injury and Disability Unit at Makerere University School of Public Health was the only unit in Uganda that focuses on research of injury and prevention.

According to Hon. Agasha, there are many unqualified drivers on Uganda’s road who commit a lot of traffic offenses and sometimes walk away without punishment due to lack of monitoring systems. She also says most drivers lack good training and that some simply acquire driving permits without ever going to the driving schools.
“If we can have the measures that can monitor whoever makes a mistake, and then they charge accordingly, I know as Ugandans, we fear fines very much. The moment they fine you today, I don’t think tomorrow you can repeat the same mistake,” says Hon. Agasha.
She advocates for more cameras to track traffic crimes in order to improve road safety. “In fact, you find someone who is driving without a seatbelt and when he senses a traffic person, that is when he remembers that seatbelts are supposed to be used. So there is a lot of effort that we have to put in in order to reduce on road accidents especially on these motorcycles. You find a big group of motorcycles driving when there are red lights and they don’t mind whether there is red or green for them they keep moving. But if they can be controlled or sensitized about dangers of a vehicle that coming from a different direction, I believe we can reduce on the road accidents,” says Hon. Agasha.
The MP for Iki-Iki County in Budaka district, Robert Kasolo agrees that using technology in enforcement of traffic order is the way to go. He expresses concern that cameras in Uganda are largely not for road traffic law enforcement but for security reasons. “But I think that would be the ideal situation. In developed countries, cameras are part of the gadgets for enforcing traffic laws. We need to move in that direction. Policemen cannot be everywhere. But a camera can record a wider area and can be a source of evidence,” says Hon. Kasolo, who also doubles as Vice Chairperson of the Physical Infrastructure Committee of Parliament.

Tonny Ayo, the Member of Parliament for Kwania County, and Vice chairperson Parliamentary committee on Road Safety wants the Uganda Police Traffic department to begin to use the cameras both within the cities and high ways to bring drivers to book.
“One of our concerns of ensuring that people follow the traffic regulations and laws is that government put in place the cameras on streets and highways and we have spent money on this and the purpose was not only to deal with crime and terrorism but one of them was enforcement of traffic rules and regulations which unfortunately as a Forum as parliament and a public are wondering why government cannot come up to enforce this,” says Hon. Ayo.

He opines that; “When you drive along highways and roads within Kampala, the reckless driving of high speed, the bad overtaking, we expected that cameras could take stock of what is happening. We are calling on government to move in to ask police to begin to use these cameras to enforce the laws.”
According to Hon. Ayo, using video and pictorial evidence from the cameras, government will go a long way in collecting huge non-tax revenue through fines of traffic offenders.
“If we do this consistently for 6 months, then we are going to see discipline by the motorist in in this country and I think by the decade plan of action we were supposed to have reduced road crashes and injuries in the country by half by 2020. Now we are in 2022, and instead of reducing, the crashes and injuries have increased. That means now we need to act because we have noticed that sensitization and talking to people,” says Hon. Ayo.
Dr. Olive Chifefe Kobusingye, an accident & emergency surgeon, injury epidemiologist at MakSPH says TRIAD’s biggest concern is road safety and accessible for all road users. She ads that this can be achieved through good road designs.
“Designing for all road users not just for motorists. Making sure that there is space to accommodate pedestrians, cyclists, motorcyclists and accommodate those that are using wheel chairs for instance and to pay attention to the size of the population so that we in the design cater for heavy pedestrian presence, those spaces are adequate for them,” says Dr. Kobusingye.

In addition to the design, Dr. Kobusingye also agrees with the legislators on the need to increase enforcement of traffic regulations in Uganda to ensure road safety.
“There are areas where we need to enforce for instance where there is limited access to motorized traffic. These are all provided for in the non-motorized transport policy. So, the implementation of that policy is key to ensuring that transportation is safe, its accessible, its affordable and that its equitable that we do not prioritize certain types of road users over others,” Dr. Kobusingye observes.

You may like
-


TORCH Project Deepens Climate Action and Sustainable Agriculture Through Community Living Lab in Kabale
-


WHO Report Highlights Global Drowning Burden as MakSPH Contributes to Evidence and Action
-


From Information to Innovation: ‘This Is a Marathon, Not a Sprint’—Academic Registrar and Director of Graduate Training Urge PhD Cohort 11
-


Call for GRANT Applications: The 2026 AAUN Partnership & Research Development Fund (PRDF)
-


Uganda and RUFORUM Cement Ties to Advance Agricultural and Academic Collaboration
-


Applications for Admission to Undergraduate Programmes 2026/27
Health
WHO Report Highlights Global Drowning Burden as MakSPH Contributes to Evidence and Action
Published
22 hours agoon
May 6, 2026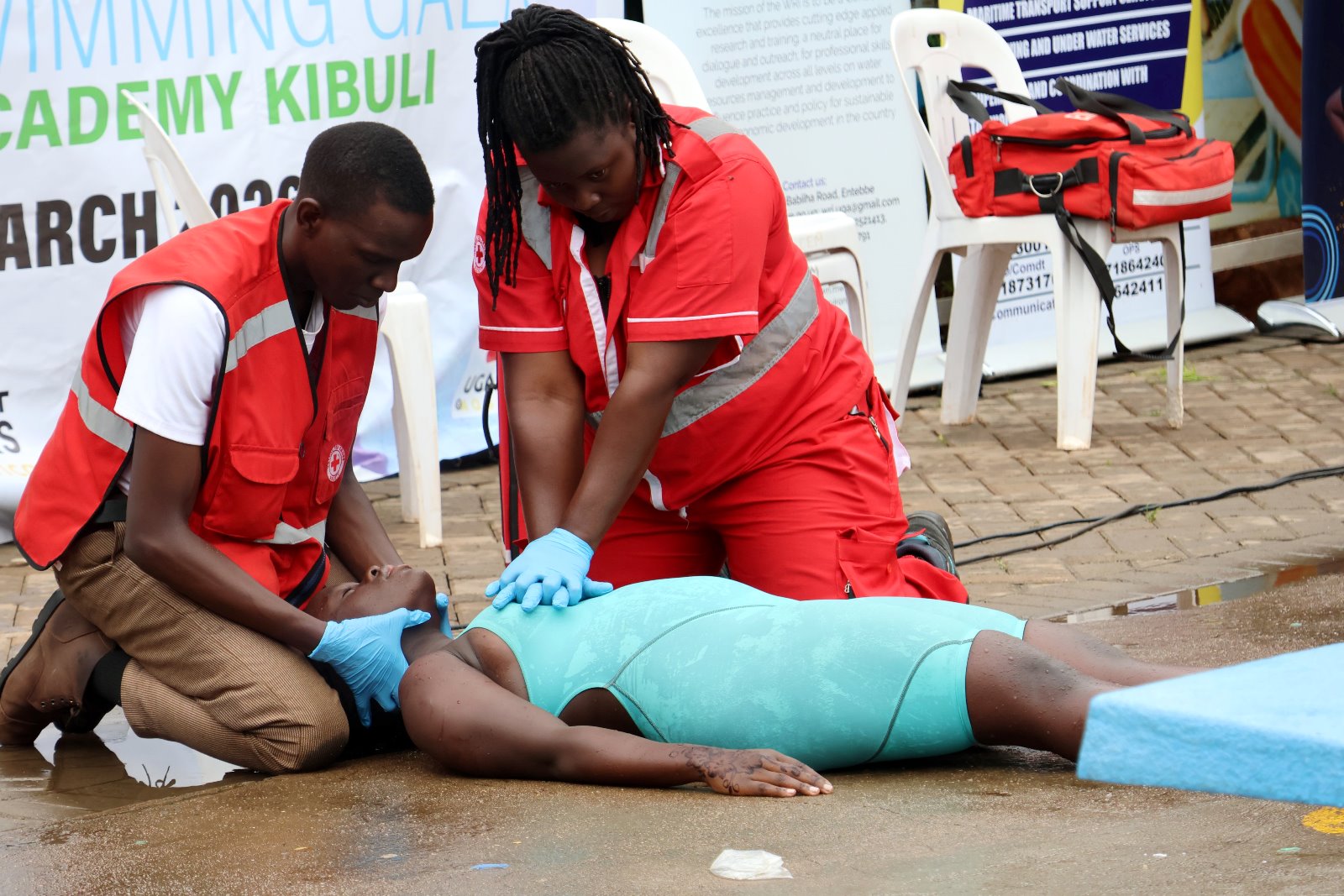
Makerere University School of Public Health, through its Centre for the Prevention of Trauma, Injury and Disability, contributed to the Global Status Report on Drowning Prevention 2024, the first comprehensive global assessment of drowning burden, risk factors, and country-level responses.
Published by the World Health Organisation, the report estimates that approximately 300,000 people died from drowning in 2021, with the highest burden in low- and middle-income countries, which account for 92% of deaths. The African Region records the highest mortality rate, underscoring the urgency of targeted interventions. Children and young people remain the most affected, with drowning ranking among the leading causes of death for those under 15 years.
While global drowning rates have declined by 38% since 2000, progress remains uneven and insufficient to meet broader development targets. The report highlights critical gaps in national responses, including limited multisectoral coordination, weak policy and legislative frameworks, and inadequate integration of key preventive measures such as swimming and water safety education.
It further identifies persistent data limitations, with many countries lacking detailed information on where and how drowning occurs, constraining the design of targeted interventions. At the same time, the report notes progress in selected areas, including early warning systems and community-based disaster risk management.
MakSPH’s contribution to this global evidence base reflects its role in advancing research, strengthening data systems, and supporting context-specific approaches to injury prevention. Through its Centre, the School continues to inform policy and practice, contributing to efforts to reduce drowning risks and improve population health outcomes in Uganda and similar settings.
The full report can be accessed below:
Health
Makerere University’s role in empowering Uganda’s Vital Statistics for CRVS Reform
Published
1 week agoon
April 27, 2026By
Mak Editor
By Dan Kajungu
In many low- and middle-income countries, mortality data remains a critical gap in public health planning, often leaving a significant portion of the population “invisible” in official records. In Uganda, where national death registration completeness has historically hovered around a mere 20%, Makerere University Centre for Health and Population Research (MUCHAP) is leading a transformative initiative. By leveraging the infrastructure of the Health and Demographic Surveillance System (HDSS), MUCHAP has demonstrated how academic research frameworks can be integrated into national systems to strengthen Civil Registration and Vital Statistics (CRVS).
A Bridge between research and governance
The core of this success lies in the collaboration between Makerere University’s infrastructure and government agencies, specifically the National Identification and Registration Authority (NIRA). This partnership, supported by the Uganda National Public Health Institute (UNPHI) and international partners like the Bloomberg Philanthropies Data for Health Initiative at the CDC Foundation, aimed at aligning local death recording practices with the legal requirements of the Registration of Persons Act (ROPA) 2015.
By utilizing the existing MUCHAP Iganga Mayuge HDSS platform, which has monitored births and deaths in the Iganga and Mayuge districts since 2005, the project demonstrated the use of a decentralized notification process. This model utilises Village Health Teams (VHTs) who already serve as HDSS scouts and part of the Ministry of Health systems as official death notifiers. These VHTs assist households in completing official NIRA notification forms at the household/community level, which are then verified by local leaders and submitted to District Registration Offices.
Impact: From 20% to over 70% completeness
The results of this collaboration have been profound. In the pilot sub counties in the districts of Iganga and Mayuge, death registration completeness reached 73–79%, a dramatic improvement over the prevailing national estimates. During the study period, 2,992 deaths were officially registered within the national CRVS system.
Key drivers of this success included:
- Reduced barriers: Decentralization brought the registration process closer to home, with an average travel distance of only 4–5 km for notification, compared to the significant distances previously required to reach district offices.
- Cost savings: Families reported that the community-based process eliminated unofficial fees and high transportation costs, facilitating essential cultural and legal tasks like property inheritance and appointing heirs.
- Advanced surveillance: The project proved that local health personnel could successfully conduct verbal autopsies (VA) in non-HDSS settings, providing critical data on causes of death that were previously unavailable for home-based deaths.
Sustainability and future potential
The MUCHAP-IMHDSS model is designed for long-term sustainability and national scalability. By embedding these tasks within the routine activities of VHTs and local leaders, the process becomes streamlined and cost-effective over time. The project also highlights that community sensitization is vital to maintaining trust and ensuring high participation rates, particularly in rural areas.
Looking forward, this initiative serves as a scalable blueprint for the rest of Uganda and other low-resource settings. Future engagements are expected to focus on:
- National scale-up: Applying the lessons learned from Iganga and Mayuge to the entire country to close the mortality surveillance data gap.
- Integration with health systems: Linking the CRVS data with broader health information systems to enhance pandemic preparedness and routine public health actions.
- Regional leadership: Aligning with the Africa CDC’s initiative to strengthen mortality surveillance across the continent, positioning Uganda’s university-led model as a regional gold standard.
The HDSS-CRVS integration Project Leader Dr. Dan Kajungu who is the Executive Director of MUCHAP emphasised that “through this work, Makerere University has again proved that academic infrastructure is not just for research, but a vital engine for building resilient national governance and health systems”. This work was disseminated at the 2026 CRVS Research Forum in Bangkok, Thailand and can be accessed at https://shorturl.at/8JLTd
Dan Kajungu Msc PhD is the Executive Director MUCHAP
Health
World Malaria Day 2026: Makerere scientists have found the countdown clock for when Ugandan children will die from malaria: The question is whether anyone is listening
Published
2 weeks agoon
April 25, 2026By
Mak Editor
On a day when the world declares it can and must end malaria, new research from Eastern Uganda shows climate change is working against us and that the evidence to fight back exists right here at home
Special Feature | World Malaria Day, 25 April 2026
By Health and Science Correspondent
Today, 25 April 2026, Uganda joins the rest of the world in marking World Malaria Day under the global theme: “Driven to End Malaria: Now We Can. Now We Must.” It is a rallying cry rooted in genuine optimism. Since 2000, 2.3 billion malaria cases and 14 million deaths have been averted globally. Forty-seven countries have been certified malaria-free, and between 2000 and 2024, the number of malaria-endemic countries fell sharply from 108 to 80.
Uganda is not one of those success stories, not yet. Malaria is endemic in 96% of Uganda, accounting for 29.1% of outpatient visits and 39.5% of hospital admissions, with over 17,556 estimated malaria deaths annually, the highest burden falling on children under five years of age. And on this World Malaria Day, a new alarm has been sounded from the heart of one of Uganda’s most malaria-burdened communities, not by foreign researchers, not by a distant global health organisation, but by scientists at Makerere University, drawing on two decades of data they have collected in the villages of Iganga and Mayuge in Eastern Uganda.
Their message is urgent: climate change is silently and measurably worsening Uganda’s malaria crisis. But this is the equally important half of the story. They have now identified the precise conditions under which children die, and exactly how long in advance those deaths can be predicted. Uganda has, for the first time, a scientifically validated early warning system for climate-driven malaria mortality. Whether the country chooses to use it is now a question of political will, not scientific capacity.
The study and the platform that made it possible
Published in BMC Public Health in August 2025, the study — “Climate-driven malaria mortality among children in malaria-endemic areas of Uganda” — was led by Dan Kajungu of Makerere University‘s Centre for Health and Population Research (MUCHAP). It analysed 14 years of weekly malaria death data from January 2008 to December 2022 matched against climate variables, using a sophisticated time-series statistical approach called the Distributed Lag Non-linear Model.
The data came from the Iganga Mayuge Health and Demographic Surveillance Site (IMHDSS), the population research platform that Makerere University has operated continuously since 2005. The IMHDSS population cohort collects data from 65 villages located within an area of 155 square kilometres, monitoring a population of close to 100,000 people. The site has 23 health facilities, including two general hospitals, and a bimodal tropical climate with rainfall seasons from March to May and September to November.
What makes the IMHDSS extraordinary and what made this study possible is its method of capturing deaths. Rather than relying on hospital registers that miss the majority of rural deaths, malaria deaths were identified using verbal autopsies and the InterVA algorithm, a probabilistic tool that uses verbal autopsy questionnaires and Bayesian statistical techniques to estimate the probabilities of various causes of death based on signs and symptoms reported by bereaved families. Three different WHO verbal autopsy tools are used, tailored for neonates, children, and adults respectively.
In other words, when a child dies in a village in Iganga, the IMHDSS knows about it. It interviews the family. It determines why the child died. And it has been doing this, without interruption, for twenty years. The result is a dataset that is both scientifically rare and profoundly Ugandan, generated here, about us, by our own researchers.
A total of 858 malaria-related deaths were recorded in the Iganga-Mayuge districts between 2008 and 2022. Of these, 53% were among males and 47% females. The vast majority, about 73% occurred among children under five years of age, while the fewest deaths occurred among those aged 15 to 49 years. Males exhibited higher mortality proportions across all age groups, except among the elderly.
Eight hundred and fifty-eight deaths. Each one a child or adult with a name, a family, a community. Each one counted.
The finding that changes everything: Uganda now has a malaria early warning system
The scientific heart of this study, the finding that every health planner, every district malaria coordinator, and every Minister of Health in Uganda should understand is this: the researchers have identified the exact temperature and rainfall thresholds at which malaria deaths among children rise, and how many weeks in advance those deaths can be predicted.
The study found an increased mortality risk across all ages at a lag of 11 to 12 weeks following exposure to rainfall above 646 mm. Higher risks of malaria mortality were also observed at a lag of 5 to 11 weeks when temperatures ranged between 25.2°C and 29.9°C. Critically, the relative risk of malaria mortality in children under five years and children aged between 5 and 14 years was more sensitive to temperature than to rainfall.
Read that again, slowly. When temperatures in Eastern Uganda climb into the range of 25.2°C to 29.9°C, children begin dying of malaria five to eleven weeks later. When extreme rainfall events exceed 646 mm, deaths rise eleven to twelve weeks after that exposure. Uganda’s meteorological service measures temperature and rainfall continuously. Uganda’s health system manages malaria interventions. These two systems have never been formally connected, but the science to connect them now exists.
This is what a malaria early warning system looks like. Not a foreign technology imported at great expense. Not a satellite system requiring international expertise to interpret. A Ugandan scientific finding, produced from Ugandan data, that tells Ugandan health authorities: when you see these weather conditions, stock your health centres, distribute your bed nets, deploy your community health workers, and prepare, because the deaths are coming in six to twelve weeks if you do not act.
On this World Malaria Day, when the global community declares that ending malaria is now possible, Uganda has precisely this tool in its hands. The only question is whether it will use it.
Climate change is not a future threat, it is already killing children
The global theme for World Malaria Day 2026 carries urgency partly because climate change, conflict, and humanitarian crises continue to drive malaria resurgence and disrupt essential services. The Makerere study puts specific, local flesh on that global warning.
Malaria is climate-sensitive, changes in temperature, rainfall patterns, and relative humidity affect the dynamics and intensity of malaria transmission by influencing the habitats of mosquitoes and parasites and their biological growth cycle. Climate remains an indirect cause of malaria mortality by affecting parasite development during periods of high rainfall and temperatures, leading to increased transmission, morbidity, and severe malaria outcomes.
The malaria parasite Plasmodium falciparum, the species responsible for almost all malaria deaths in Uganda requires specific temperature ranges to complete its development inside the Anopheles mosquito. Too cold, and development slows or stops. Too hot, and it also stops. But within the range that Eastern Uganda increasingly inhabits, and will inhabit more frequently as global temperatures rise, the parasite thrives, multiplies, and kills.
The World Malaria Report 2025 warns that drug resistance is now confirmed in four African countries including Uganda, where artemisinin partial resistance has been detected. Insecticide resistance to pyrethroids – the main chemical on bed nets is now confirmed in 48 out of 53 reporting countries. As the tools Uganda currently relies on including bed nets, indoor spraying, artemisinin-based drugs face mounting biological resistance, the importance of climate-informed prevention strategies grows exponentially. Deploying interventions at exactly the right time, guided by weather data, becomes not just efficient but essential.
The children most at risk: a finding that demands a policy response
Among the study’s most striking findings is the specific vulnerability of school-age boys. A group almost entirely absent from Uganda’s current malaria prevention architecture.
Male children aged between 5 and 14 years were found to be more vulnerable to temperature-related malaria mortality compared to females in that age group and compared to children under five years. Rainfall did not have a significant association with malaria mortality in children.
Uganda’s National Malaria Control Programme, like most in sub-Saharan Africa, has historically concentrated resources on two priority groups: children under five and pregnant women. These groups are undeniably vulnerable and deserve protection. But this study shows that school-age boys are dying from temperature-driven malaria at rates that demand their inclusion in prevention strategies.
School-aged children between 5 and 14 years have higher malaria prevalence, with 70% carrying the malaria parasite asymptomatically in high transmission settings. They carry the parasite silently, sustaining transmission in their communities, and they die when temperatures rise, particularly the boys, who in rural Uganda spend more time outdoors, sleep less consistently under nets, and receive less parental health supervision than their sisters as they grow older.
The study’s area is itself among the most heavily burdened in Uganda. The Iganga-Mayuge area has a malaria prevalence rate of 39.4% in children under five years old, making it one of the areas in Uganda most severely impacted by malaria, and the disease is the leading cause of mortality in children there. In such a high-transmission setting, the combination of asymptomatic carriage, temperature-driven transmission spikes, and inadequate prevention coverage for school-age children is a formula for preventable death.
On World Malaria Day 2026, as Uganda declares its commitment to ending malaria, the national malaria strategy must be updated to reflect this evidence. School-based distribution of insecticide-treated nets, school health programmes that include malaria education and early symptom recognition, and targeted community outreach for families with boys aged 5 to 14 are not optional additions, they are evidence-based necessities.
The platform: Makerere‘s IMHDSS as a national asset for malaria elimination
None of the findings in this study would have been possible without the IMHDSS and on World Malaria Day, it is worth being explicit about what that platform represents for Uganda’s future.
The IMHDSS platform has measured various indicators about coverage and uptake of national interventions including the coverage and utilisation of immunisation and vaccines, mosquito nets for malaria vector control, household income improvement, and family planning, and other behaviour change interventions at community level, strengthening the evaluation of burden of disease at the subnational level.
For malaria specifically, the IMHDSS has now produced the most granular mortality data in Uganda’s history capturing not just how many children die, but exactly which weather conditions preceded those deaths, which sex and age group is most vulnerable, and what the biological and epidemiological mechanisms are that connect climate to the grave. This is the kind of intelligence that a National Malaria Control Programme needs to move from reactive crisis management to proactive, evidence-driven prevention.
Scarcity of quality data remains a key development bottleneck in low and middle-income countries, and the Iganga-Mayuge HDSS represents a Makerere University platform for research and research training with a population-based cohort that longitudinally generates data for evidence-based decisions and policy.
Uganda’s malaria elimination goal, to bring mortality to zero will not be achieved by effort and goodwill alone. It requires data. It requires the kind of longitudinal, community-level, cause-of-death data that only a platform like the IMHDSS can generate. And it requires the institutional will to connect that data to the decisions that determine whether children live or die.
What must happen now
The global call on World Malaria Day 2026 is clear: “Now We Can. Now We Must.” For Uganda, the Makerere climate-malaria study translates that call into three specific and achievable actions.
First, the Ministry of Health and Uganda National Meteorological Authority must establish a formal, operational malaria early warning system. One that uses real-time weather monitoring to trigger predetermined health system responses when temperature and rainfall thresholds identified by this research are breached. The science is ready. The infrastructure for meteorological monitoring exists. What is needed is the institutional bridge between them.
Second, Uganda’s National Malaria Control Programme must extend its prevention focus to include school-age children, particularly boys aged 5 to 14, in all high-transmission areas. Bed net campaigns must reach schools, not just health centres and antenatal clinics. Community health workers must be equipped to identify and treat malaria in this age group as a priority.
Third, and most fundamentally, the Government of Uganda must formally recognise and domestically resource the IMHDSS as national public health infrastructure. The 2024 global malaria funding of US$3.9 billion was less than half of the US$9.3 billion target, leaving a projected shortfall of US$5.4 billion that leaves the response dangerously under-resourced. In a world where international health financing is under historic pressure, Uganda cannot afford to have its most powerful evidence-generation platform dependent entirely on foreign philanthropy. The IMHDSS is a Ugandan asset. It must be funded as one.
Today, children in Iganga and Mayuge are alive who might not be, because the research generated by the IMHDSS informed the malaria interventions that reached their communities. Today, Makerere scientists have given Uganda a tool, a climate-based early warning system for malaria deaths that no other country in East Africa currently possesses.
Now we can. Now we must.
The evidence is there. The science is done. The only thing Uganda needs now is the will to act on it.
“Climate-driven malaria mortality among children in malaria-endemic areas of Uganda” is published open-access in BMC Public Health, Volume 25, Article 2825, August 2025. Full text available at: https://link.springer.com/article/10.1186/s12889-025-23678-0
The Iganga Mayuge Health and Demographic Surveillance Site (IMHDSS) is operated by MUCHAP, Makerere University. Contact: info@muchap.mak.ac.ug or dkajungu@muchap.mak.ac.ug| Tel: +256 772 207127 (Dr. Dan Kajungu)
Trending
-

 General1 week ago
General1 week agoApplications for Admission to Undergraduate Programmes 2026/27
-

 General2 weeks ago
General2 weeks agoNational Merit Scholarship Undergraduate Admission List 2026/2027
-

 Agriculture & Environment1 week ago
Agriculture & Environment1 week agoRe-Advertised Call for Applications: QCF Postdoctoral Research Fellowships
-

 General1 week ago
General1 week agoDiploma Holders Admission Lists under Government Sponsorship for 2026/2027 AY
-

 Research2 weeks ago
Research2 weeks agoMakerere Revives Scholarly Publishing through Journal Editors’ Workshop to Boost Global Rankings
