Health
Inside Uganda’s National Health Adaptation Plan to Combat Climate Change
Published
2 years agoon
By
Mak Editor
By John Okeya
On August 22, 2024, Uganda made history as the first African nation to launch a National Health Adaptation Plan (H-NAP), fulfilling the country’s global commitments at the UN Conference of Parties (COP) 26 and 28 summits in Glasgow (2021), and Dubai (2023), respectively, in response to the growing global climate change risks and challenges.
The National Health Adaptation Plan 2025-2030, dubbed H-NAP, which was launched by the health ministry yesterday in Kampala, seeks to fortify the country’s healthcare system against the current mounting health challenges driven by climate fluctuations, to safeguard public well-being amid the rising temperatures, erratic weather patterns, and associated health risks.
Officiating the H-NAP launch, Uganda’s Prime Minister, Rt. Hon. Robinah Nabbanja, represented by the third Deputy Prime Minister and Minister without Portfolio, Rt. Hon. Lukia Isanga Nakadama, commended the fruitful collaborative initiative of the government, development, and civil society partners in delivering the Health National Adaptation Plan.
“The government of Uganda has created an enabling policy and legal environment to tackle the climate change challenges,” she noted emphatically, revealing that: “In the Parish Development Model (PDM), we need to integrate climate change interventions. I was recently talking to my people (constituents in Mayuge district) about the PDM programme, I told them; ‘we gave you money and we know you are doing well. They said no, all our crops were washed away by the heavy rains, we did not get anything.’ So, it’s not all that easy.”

She said the current five-year term National Development Plan (NDP) III which is bound to expire and the new NDP IV underscore climate change as a cross-cutting issue requiring mainstreaming across all sectors, assuring that the Office of the Prime Minister (OPM) will coordinate multisectoral engagements for Ministries, Departments, and Agencies (MDAs) and support awareness raising for the new Health National Adaptation Plan.
“I congratulate the Ministry of Health and all sectoral partners for developing the Health National Adaptation Plan that we are launching today. This Plan is based on evidence from the Climate Change Health Vulnerability and Adaptation Assessment and should provide a systematic guide to building a resilient health system for Uganda,” the Prime Minister observed, urging the different multi-stakeholders to support the implementation of the Plan to harness its full potential in guiding the country’s climate change adaptation action.
Climate change adaptation, commonly used, means the steps taken to help both natural and human environmental systems adjust to the impacts of climate change, whether those changes are happening now or expected in the future. Such interventions may include actions, policies, and strategies designed to specifically reduce the negative effects of climate change while making the most of any potential benefits that may arise.
On the other hand, climate change refers to the long-term shifts in temperatures and weather patterns, mostly caused by human activities like burning fossil fuels, which release greenhouse gases (also known as GHGs) into the atmosphere. These changes lead to more extreme weather events, rising sea levels, and ecosystem disruptions, impacting everything, from agriculture to human health.
One of the key successes arising out of the two weeks deliberation between 120 world leaders and over 40,000 registered participants, including 22,274 party delegates, 14,124 observers, and 3,886 media representatives at COP26 summit in Glasgow, from Sun, Oct 31, 2021 – Fri, Nov 12, 2021, was the compromise to step up support for climate change adaptation, reflected in the Glasgow Pact calling for the doubling of finance to support developing countries like Uganda in adapting to the adverse weather impacts and build resilient health systems.
A key highlight during the Glasgow negotiations, was the realisation by the global actors of the critical linkage between climate change and health, as the discussions culminated in the consensus that the worsening climate crisis directly threatens global health through increased extreme weather events, the spread of diseases, and the increased strain on healthcare systems, thus necessitating urgent integrated action to protect public health.
Subsequently, nation states committed to developing national climate change health vulnerability and adaptation assessments and the health national adaptation plans, both documents that Uganda has now concluded, to emerge as a regional and global leader in the charge towards adaptation to combat climate change effects and build resilience.
The November 2023 Climate Change Health Vulnerability and Adaptation Assessment (VAA) for Sound Management of Climate Change-related Health Risks in Uganda and the Health – National Adaptation Plan (H-NAP) 2025- 2030, were conducted through a collaboration led by Uganda’s Ministry of Health, with partners including Rockefeller Foundation, Makerere University, World Health Organization, Ministry of Water and Environment, Amref Health Africa, Reproductive Health Uganda, Pathfinder Uganda, Tree Adoption Uganda, Seed Global Health Uganda, Clinton Health Access Initiative and Regenerate Africa.
Makerere University School of Public Health’s Dr. John Bosco Isunju, who led the teams in the development of both the VAA and H-NAP, was honoured by the Ministry of Health with the 2024 Climate and Health Champions Award during the Health National Adaptation Plan Launch, for his significant contributions to building a climate-resilient health system in Uganda.

The Rockefeller Foundation’s investment played a pivotal role in funding the development of these two strategic documents. Mr. William Asiko, Vice President and head of The Rockefeller Foundation’s Africa Regional Office, emphasised, “Climate change is now the gravest threat to the health and well-being of billions of African people. Initiatives like Uganda’s Health National Adaptation Plan demonstrate how African countries are rising to the challenge by scaling the necessary climate solutions and setting an example for the world.”

Makerere University Vice Chancellor, Prof. Barnabas Nawangwe, in his remarks delivered by the University Secretary, Mr. Yusuf Kiranda commended the role played by the partners in the development of the Plan, noting that: “Our academics from the Makerere University School of Public Health played a vital role in leading the Climate Change Vulnerability and Adaptation Assessment (VAA), which has been instrumental in shaping the development of the H-NAP.”
“This is just one example of Makerere University’s strategic commitment to research, innovation, and capacity-building. We are dedicated to generating evidence and human resources capabilities that guide decision-making and contribute to the development and implementation of climate-resilient strategies in health, agriculture, and other sectors,” the Makerere University Vice Chancellor observed.
He stated that the success of the National Adaptation Plan depends on the strength of our collaborations, which requires concerted efforts of government ministries, health agencies, civil society organisations, the private sector, development partners, and the academic community, as he reiterated University’s commitment to being a key partner in the endeavour.

Today, Uganda, like the rest of the region and the globe, continues to grapple with the adverse effects of climate change. Subsequently, the Health National Adaptation Plan’s overarching goal is to enhance the resilience of Uganda’s health sector against climate-related impacts by incorporating climate adaptation into health strategies and planning, ensuring sustainable and continuous healthcare services during climatic challenges;
“Uganda is already experiencing severe climate change effects, such as floods, droughts, and temperature changes, which contribute to health issues like waterborne diseases, vector-borne diseases, malnutrition, and mental health problems.” The H-NAP report reads in part.
Its precursor, the 2023 Climate Change Health Vulnerability and Adaptation Assessment (VAA) survey, conducted across 716 selected health facilities in Uganda, highlighted the significant risks and challenges that climate change poses to public health.
The Vulnerability Assessment revealed that many healthcare facilities in Uganda are highly vulnerable to climate change-related hazards, due to unpreparedness across several critical components. In terms of energy, healthcare facilities were found to lack secure locations to protect emergency energy sources from hazards, had inadequate coverage for critical service areas, and failed to consistently check alternative energy sources.
The health workforce was also underprepared, with gaps in participation in climate adaptation plans, insufficient readiness for outdoor work during extreme conditions, and limited capacity to identify and manage health conditions, worsened by climate impacts.
Significant weaknesses were apparent in water, sanitation and hygiene, and healthcare waste management, including inadequate strategies to monitor and reduce water contamination, limited preparedness to prevent vector breeding in facility water systems, and a lack of comprehensive water safety and contingency plans. Post-hazard recovery plans were insufficient, with no safe locations for critical equipment during emergencies, inadequate safety measures for vital supplies, and inconsistent evacuation mechanisms for health workers and patients.
“These findings highlight a need for implementation of climate change adaptation plans and policies, building capacity of the health workers, and strengthening WASH management systems and water safety plans. There’s also a need for improvement of the reliability of energy infrastructure, development of contingency plans and enhancement of infrastructure resilience, evacuation plans, and post-disaster recovery,” the VAA report reads in part.
Today, Uganda has established a robust policy and legal framework to address climate change, including the National Climate Change Policy of 2015, the Climate Change Act of 2021, and the updated Nationally Determined Contribution of 2022. These frameworks aim to transform Uganda into a climate-resilient, low-carbon society by 2050.
The Uganda National Health Adaptation Plan (H-NAP) aligns with these policies, emphasising the integration of climate change adaptation into health sector plans and policies.
“A key recommendation to tackle climate change issues in Uganda is the integration of climate services for health. These services involve the provision of climate data, tools, and information tailored to the health sector’s needs, enabling health professionals to better anticipate, prepare for, and respond to climate-related health risks. Climate services for health include forecasting climate variables, monitoring and predicting the spread of climate-sensitive diseases and issuing early warnings for heatwaves and air pollution episodes,” The H-NAP reads in part.
According to the Plan, by integrating these services into health planning and operations, Uganda can enhance its public health resilience against the impacts of climate change. Furthermore, the H-NAP proposes a range of short-term and long-term interventions across ten components that include climate-transformative leadership, climate-smart health workforce, integrated risk monitoring, and sustainable financing.
From the H-NAP, specific actions identified include developing guidelines for mainstreaming climate and health, training health workers, enhancing disease surveillance systems, and revising infrastructure standards for climate-proofing. Also, the plan presents a financing framework to mobilise resources for implementing the identified interventions. This includes developing a comprehensive resource mobilisation plan, increasing national budgets for health and climate change policies, and advocating for health issues in climate funding streams.
Uganda is all too familiar with the harsh realities of climate change, having continuously experienced rising temperatures, prolonged droughts, and increasingly severe rainy seasons—each intensifying public health challenges. This National Health Adaptation Plan marks a critical step in the country’s climate action efforts, standing as the first of its kind. It serves as a crucial component of Uganda’s broader strategy to mitigate climate impacts and safeguard public health in the face of growing environmental threats.
You may like
-


Making Waves: The Rise of the Mak Sharks and Makerere University’s Aquatic Legacy
-


Press Release: Government of Uganda and Partners Launch SAY Plus+ to Scale Youth Sexual Reproductive Health & Rights (SRHR) Impact in Underserved Regions
-


TORCH Project Deepens Climate Action and Sustainable Agriculture Through Community Living Lab in Kabale
-


WHO Report Highlights Global Drowning Burden as MakSPH Contributes to Evidence and Action
-


From Information to Innovation: ‘This Is a Marathon, Not a Sprint’—Academic Registrar and Director of Graduate Training Urge PhD Cohort 11
-


Uganda and RUFORUM Cement Ties to Advance Agricultural and Academic Collaboration
Health
WHO Report Highlights Global Drowning Burden as MakSPH Contributes to Evidence and Action
Published
2 days agoon
May 6, 2026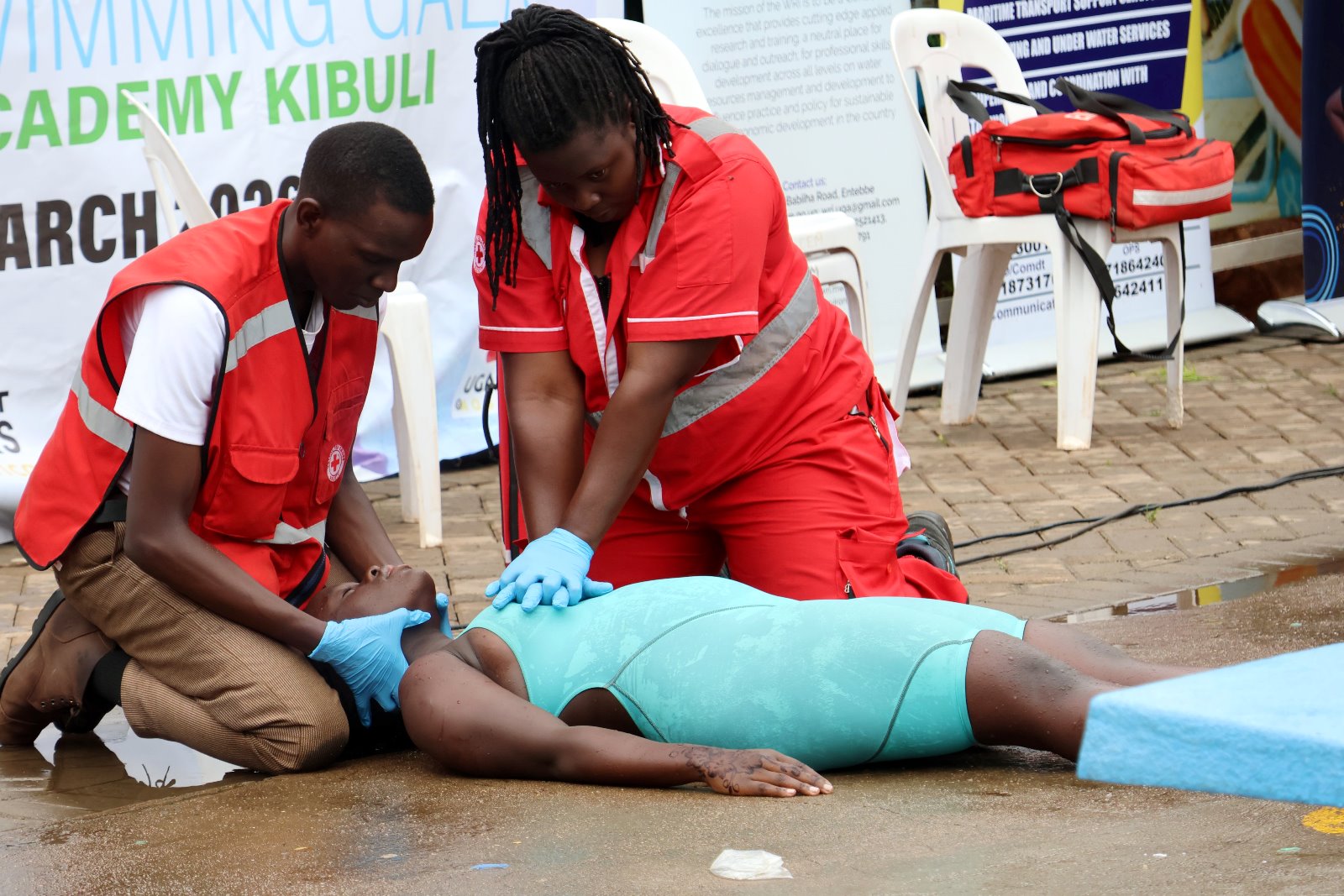
Makerere University School of Public Health, through its Centre for the Prevention of Trauma, Injury and Disability, contributed to the Global Status Report on Drowning Prevention 2024, the first comprehensive global assessment of drowning burden, risk factors, and country-level responses.
Published by the World Health Organisation, the report estimates that approximately 300,000 people died from drowning in 2021, with the highest burden in low- and middle-income countries, which account for 92% of deaths. The African Region records the highest mortality rate, underscoring the urgency of targeted interventions. Children and young people remain the most affected, with drowning ranking among the leading causes of death for those under 15 years.
While global drowning rates have declined by 38% since 2000, progress remains uneven and insufficient to meet broader development targets. The report highlights critical gaps in national responses, including limited multisectoral coordination, weak policy and legislative frameworks, and inadequate integration of key preventive measures such as swimming and water safety education.
It further identifies persistent data limitations, with many countries lacking detailed information on where and how drowning occurs, constraining the design of targeted interventions. At the same time, the report notes progress in selected areas, including early warning systems and community-based disaster risk management.
MakSPH’s contribution to this global evidence base reflects its role in advancing research, strengthening data systems, and supporting context-specific approaches to injury prevention. Through its Centre, the School continues to inform policy and practice, contributing to efforts to reduce drowning risks and improve population health outcomes in Uganda and similar settings.
The full report can be accessed below:
Health
Makerere University’s role in empowering Uganda’s Vital Statistics for CRVS Reform
Published
2 weeks agoon
April 27, 2026By
Mak Editor
By Dan Kajungu
In many low- and middle-income countries, mortality data remains a critical gap in public health planning, often leaving a significant portion of the population “invisible” in official records. In Uganda, where national death registration completeness has historically hovered around a mere 20%, Makerere University Centre for Health and Population Research (MUCHAP) is leading a transformative initiative. By leveraging the infrastructure of the Health and Demographic Surveillance System (HDSS), MUCHAP has demonstrated how academic research frameworks can be integrated into national systems to strengthen Civil Registration and Vital Statistics (CRVS).
A Bridge between research and governance
The core of this success lies in the collaboration between Makerere University’s infrastructure and government agencies, specifically the National Identification and Registration Authority (NIRA). This partnership, supported by the Uganda National Public Health Institute (UNPHI) and international partners like the Bloomberg Philanthropies Data for Health Initiative at the CDC Foundation, aimed at aligning local death recording practices with the legal requirements of the Registration of Persons Act (ROPA) 2015.
By utilizing the existing MUCHAP Iganga Mayuge HDSS platform, which has monitored births and deaths in the Iganga and Mayuge districts since 2005, the project demonstrated the use of a decentralized notification process. This model utilises Village Health Teams (VHTs) who already serve as HDSS scouts and part of the Ministry of Health systems as official death notifiers. These VHTs assist households in completing official NIRA notification forms at the household/community level, which are then verified by local leaders and submitted to District Registration Offices.
Impact: From 20% to over 70% completeness
The results of this collaboration have been profound. In the pilot sub counties in the districts of Iganga and Mayuge, death registration completeness reached 73–79%, a dramatic improvement over the prevailing national estimates. During the study period, 2,992 deaths were officially registered within the national CRVS system.
Key drivers of this success included:
- Reduced barriers: Decentralization brought the registration process closer to home, with an average travel distance of only 4–5 km for notification, compared to the significant distances previously required to reach district offices.
- Cost savings: Families reported that the community-based process eliminated unofficial fees and high transportation costs, facilitating essential cultural and legal tasks like property inheritance and appointing heirs.
- Advanced surveillance: The project proved that local health personnel could successfully conduct verbal autopsies (VA) in non-HDSS settings, providing critical data on causes of death that were previously unavailable for home-based deaths.
Sustainability and future potential
The MUCHAP-IMHDSS model is designed for long-term sustainability and national scalability. By embedding these tasks within the routine activities of VHTs and local leaders, the process becomes streamlined and cost-effective over time. The project also highlights that community sensitization is vital to maintaining trust and ensuring high participation rates, particularly in rural areas.
Looking forward, this initiative serves as a scalable blueprint for the rest of Uganda and other low-resource settings. Future engagements are expected to focus on:
- National scale-up: Applying the lessons learned from Iganga and Mayuge to the entire country to close the mortality surveillance data gap.
- Integration with health systems: Linking the CRVS data with broader health information systems to enhance pandemic preparedness and routine public health actions.
- Regional leadership: Aligning with the Africa CDC’s initiative to strengthen mortality surveillance across the continent, positioning Uganda’s university-led model as a regional gold standard.
The HDSS-CRVS integration Project Leader Dr. Dan Kajungu who is the Executive Director of MUCHAP emphasised that “through this work, Makerere University has again proved that academic infrastructure is not just for research, but a vital engine for building resilient national governance and health systems”. This work was disseminated at the 2026 CRVS Research Forum in Bangkok, Thailand and can be accessed at https://shorturl.at/8JLTd
Dan Kajungu Msc PhD is the Executive Director MUCHAP
Health
World Malaria Day 2026: Makerere scientists have found the countdown clock for when Ugandan children will die from malaria: The question is whether anyone is listening
Published
2 weeks agoon
April 25, 2026By
Mak Editor
On a day when the world declares it can and must end malaria, new research from Eastern Uganda shows climate change is working against us and that the evidence to fight back exists right here at home
Special Feature | World Malaria Day, 25 April 2026
By Health and Science Correspondent
Today, 25 April 2026, Uganda joins the rest of the world in marking World Malaria Day under the global theme: “Driven to End Malaria: Now We Can. Now We Must.” It is a rallying cry rooted in genuine optimism. Since 2000, 2.3 billion malaria cases and 14 million deaths have been averted globally. Forty-seven countries have been certified malaria-free, and between 2000 and 2024, the number of malaria-endemic countries fell sharply from 108 to 80.
Uganda is not one of those success stories, not yet. Malaria is endemic in 96% of Uganda, accounting for 29.1% of outpatient visits and 39.5% of hospital admissions, with over 17,556 estimated malaria deaths annually, the highest burden falling on children under five years of age. And on this World Malaria Day, a new alarm has been sounded from the heart of one of Uganda’s most malaria-burdened communities, not by foreign researchers, not by a distant global health organisation, but by scientists at Makerere University, drawing on two decades of data they have collected in the villages of Iganga and Mayuge in Eastern Uganda.
Their message is urgent: climate change is silently and measurably worsening Uganda’s malaria crisis. But this is the equally important half of the story. They have now identified the precise conditions under which children die, and exactly how long in advance those deaths can be predicted. Uganda has, for the first time, a scientifically validated early warning system for climate-driven malaria mortality. Whether the country chooses to use it is now a question of political will, not scientific capacity.
The study and the platform that made it possible
Published in BMC Public Health in August 2025, the study — “Climate-driven malaria mortality among children in malaria-endemic areas of Uganda” — was led by Dan Kajungu of Makerere University‘s Centre for Health and Population Research (MUCHAP). It analysed 14 years of weekly malaria death data from January 2008 to December 2022 matched against climate variables, using a sophisticated time-series statistical approach called the Distributed Lag Non-linear Model.
The data came from the Iganga Mayuge Health and Demographic Surveillance Site (IMHDSS), the population research platform that Makerere University has operated continuously since 2005. The IMHDSS population cohort collects data from 65 villages located within an area of 155 square kilometres, monitoring a population of close to 100,000 people. The site has 23 health facilities, including two general hospitals, and a bimodal tropical climate with rainfall seasons from March to May and September to November.
What makes the IMHDSS extraordinary and what made this study possible is its method of capturing deaths. Rather than relying on hospital registers that miss the majority of rural deaths, malaria deaths were identified using verbal autopsies and the InterVA algorithm, a probabilistic tool that uses verbal autopsy questionnaires and Bayesian statistical techniques to estimate the probabilities of various causes of death based on signs and symptoms reported by bereaved families. Three different WHO verbal autopsy tools are used, tailored for neonates, children, and adults respectively.
In other words, when a child dies in a village in Iganga, the IMHDSS knows about it. It interviews the family. It determines why the child died. And it has been doing this, without interruption, for twenty years. The result is a dataset that is both scientifically rare and profoundly Ugandan, generated here, about us, by our own researchers.
A total of 858 malaria-related deaths were recorded in the Iganga-Mayuge districts between 2008 and 2022. Of these, 53% were among males and 47% females. The vast majority, about 73% occurred among children under five years of age, while the fewest deaths occurred among those aged 15 to 49 years. Males exhibited higher mortality proportions across all age groups, except among the elderly.
Eight hundred and fifty-eight deaths. Each one a child or adult with a name, a family, a community. Each one counted.
The finding that changes everything: Uganda now has a malaria early warning system
The scientific heart of this study, the finding that every health planner, every district malaria coordinator, and every Minister of Health in Uganda should understand is this: the researchers have identified the exact temperature and rainfall thresholds at which malaria deaths among children rise, and how many weeks in advance those deaths can be predicted.
The study found an increased mortality risk across all ages at a lag of 11 to 12 weeks following exposure to rainfall above 646 mm. Higher risks of malaria mortality were also observed at a lag of 5 to 11 weeks when temperatures ranged between 25.2°C and 29.9°C. Critically, the relative risk of malaria mortality in children under five years and children aged between 5 and 14 years was more sensitive to temperature than to rainfall.
Read that again, slowly. When temperatures in Eastern Uganda climb into the range of 25.2°C to 29.9°C, children begin dying of malaria five to eleven weeks later. When extreme rainfall events exceed 646 mm, deaths rise eleven to twelve weeks after that exposure. Uganda’s meteorological service measures temperature and rainfall continuously. Uganda’s health system manages malaria interventions. These two systems have never been formally connected, but the science to connect them now exists.
This is what a malaria early warning system looks like. Not a foreign technology imported at great expense. Not a satellite system requiring international expertise to interpret. A Ugandan scientific finding, produced from Ugandan data, that tells Ugandan health authorities: when you see these weather conditions, stock your health centres, distribute your bed nets, deploy your community health workers, and prepare, because the deaths are coming in six to twelve weeks if you do not act.
On this World Malaria Day, when the global community declares that ending malaria is now possible, Uganda has precisely this tool in its hands. The only question is whether it will use it.
Climate change is not a future threat, it is already killing children
The global theme for World Malaria Day 2026 carries urgency partly because climate change, conflict, and humanitarian crises continue to drive malaria resurgence and disrupt essential services. The Makerere study puts specific, local flesh on that global warning.
Malaria is climate-sensitive, changes in temperature, rainfall patterns, and relative humidity affect the dynamics and intensity of malaria transmission by influencing the habitats of mosquitoes and parasites and their biological growth cycle. Climate remains an indirect cause of malaria mortality by affecting parasite development during periods of high rainfall and temperatures, leading to increased transmission, morbidity, and severe malaria outcomes.
The malaria parasite Plasmodium falciparum, the species responsible for almost all malaria deaths in Uganda requires specific temperature ranges to complete its development inside the Anopheles mosquito. Too cold, and development slows or stops. Too hot, and it also stops. But within the range that Eastern Uganda increasingly inhabits, and will inhabit more frequently as global temperatures rise, the parasite thrives, multiplies, and kills.
The World Malaria Report 2025 warns that drug resistance is now confirmed in four African countries including Uganda, where artemisinin partial resistance has been detected. Insecticide resistance to pyrethroids – the main chemical on bed nets is now confirmed in 48 out of 53 reporting countries. As the tools Uganda currently relies on including bed nets, indoor spraying, artemisinin-based drugs face mounting biological resistance, the importance of climate-informed prevention strategies grows exponentially. Deploying interventions at exactly the right time, guided by weather data, becomes not just efficient but essential.
The children most at risk: a finding that demands a policy response
Among the study’s most striking findings is the specific vulnerability of school-age boys. A group almost entirely absent from Uganda’s current malaria prevention architecture.
Male children aged between 5 and 14 years were found to be more vulnerable to temperature-related malaria mortality compared to females in that age group and compared to children under five years. Rainfall did not have a significant association with malaria mortality in children.
Uganda’s National Malaria Control Programme, like most in sub-Saharan Africa, has historically concentrated resources on two priority groups: children under five and pregnant women. These groups are undeniably vulnerable and deserve protection. But this study shows that school-age boys are dying from temperature-driven malaria at rates that demand their inclusion in prevention strategies.
School-aged children between 5 and 14 years have higher malaria prevalence, with 70% carrying the malaria parasite asymptomatically in high transmission settings. They carry the parasite silently, sustaining transmission in their communities, and they die when temperatures rise, particularly the boys, who in rural Uganda spend more time outdoors, sleep less consistently under nets, and receive less parental health supervision than their sisters as they grow older.
The study’s area is itself among the most heavily burdened in Uganda. The Iganga-Mayuge area has a malaria prevalence rate of 39.4% in children under five years old, making it one of the areas in Uganda most severely impacted by malaria, and the disease is the leading cause of mortality in children there. In such a high-transmission setting, the combination of asymptomatic carriage, temperature-driven transmission spikes, and inadequate prevention coverage for school-age children is a formula for preventable death.
On World Malaria Day 2026, as Uganda declares its commitment to ending malaria, the national malaria strategy must be updated to reflect this evidence. School-based distribution of insecticide-treated nets, school health programmes that include malaria education and early symptom recognition, and targeted community outreach for families with boys aged 5 to 14 are not optional additions, they are evidence-based necessities.
The platform: Makerere‘s IMHDSS as a national asset for malaria elimination
None of the findings in this study would have been possible without the IMHDSS and on World Malaria Day, it is worth being explicit about what that platform represents for Uganda’s future.
The IMHDSS platform has measured various indicators about coverage and uptake of national interventions including the coverage and utilisation of immunisation and vaccines, mosquito nets for malaria vector control, household income improvement, and family planning, and other behaviour change interventions at community level, strengthening the evaluation of burden of disease at the subnational level.
For malaria specifically, the IMHDSS has now produced the most granular mortality data in Uganda’s history capturing not just how many children die, but exactly which weather conditions preceded those deaths, which sex and age group is most vulnerable, and what the biological and epidemiological mechanisms are that connect climate to the grave. This is the kind of intelligence that a National Malaria Control Programme needs to move from reactive crisis management to proactive, evidence-driven prevention.
Scarcity of quality data remains a key development bottleneck in low and middle-income countries, and the Iganga-Mayuge HDSS represents a Makerere University platform for research and research training with a population-based cohort that longitudinally generates data for evidence-based decisions and policy.
Uganda’s malaria elimination goal, to bring mortality to zero will not be achieved by effort and goodwill alone. It requires data. It requires the kind of longitudinal, community-level, cause-of-death data that only a platform like the IMHDSS can generate. And it requires the institutional will to connect that data to the decisions that determine whether children live or die.
What must happen now
The global call on World Malaria Day 2026 is clear: “Now We Can. Now We Must.” For Uganda, the Makerere climate-malaria study translates that call into three specific and achievable actions.
First, the Ministry of Health and Uganda National Meteorological Authority must establish a formal, operational malaria early warning system. One that uses real-time weather monitoring to trigger predetermined health system responses when temperature and rainfall thresholds identified by this research are breached. The science is ready. The infrastructure for meteorological monitoring exists. What is needed is the institutional bridge between them.
Second, Uganda’s National Malaria Control Programme must extend its prevention focus to include school-age children, particularly boys aged 5 to 14, in all high-transmission areas. Bed net campaigns must reach schools, not just health centres and antenatal clinics. Community health workers must be equipped to identify and treat malaria in this age group as a priority.
Third, and most fundamentally, the Government of Uganda must formally recognise and domestically resource the IMHDSS as national public health infrastructure. The 2024 global malaria funding of US$3.9 billion was less than half of the US$9.3 billion target, leaving a projected shortfall of US$5.4 billion that leaves the response dangerously under-resourced. In a world where international health financing is under historic pressure, Uganda cannot afford to have its most powerful evidence-generation platform dependent entirely on foreign philanthropy. The IMHDSS is a Ugandan asset. It must be funded as one.
Today, children in Iganga and Mayuge are alive who might not be, because the research generated by the IMHDSS informed the malaria interventions that reached their communities. Today, Makerere scientists have given Uganda a tool, a climate-based early warning system for malaria deaths that no other country in East Africa currently possesses.
Now we can. Now we must.
The evidence is there. The science is done. The only thing Uganda needs now is the will to act on it.
“Climate-driven malaria mortality among children in malaria-endemic areas of Uganda” is published open-access in BMC Public Health, Volume 25, Article 2825, August 2025. Full text available at: https://link.springer.com/article/10.1186/s12889-025-23678-0
The Iganga Mayuge Health and Demographic Surveillance Site (IMHDSS) is operated by MUCHAP, Makerere University. Contact: info@muchap.mak.ac.ug or dkajungu@muchap.mak.ac.ug| Tel: +256 772 207127 (Dr. Dan Kajungu)
Trending
-

 General1 week ago
General1 week agoApplications for Admission to Undergraduate Programmes 2026/27
-

 Agriculture & Environment2 weeks ago
Agriculture & Environment2 weeks agoRe-Advertised Call for Applications: QCF Postdoctoral Research Fellowships
-

 General1 week ago
General1 week agoDiploma Holders Admission Lists under Government Sponsorship for 2026/2027 AY
-

 Education1 week ago
Education1 week agoProf. Senteza Kajubi Fulbright Lecture Re-ignites debate on learner-centred reforms
-

 Education1 week ago
Education1 week agoSpecial University Entry Examinations for the Diploma in Performing Arts 2026/27
