Health
Mak Researchers Partner with Safe Bangle Technologies to Roll out a Real-Time Domestic Violence Reporting Bracelet
Published
2 years agoon
By
Mak Editor
By Joseph Odoi
A Consortium of Researchers from Makerere University School of Public Health/Resilient Africa Network (MakSPH/RAN), Medical College of Wisconsin (MCW), Somero Uganda together with Safe Bangle Technologies have rolled out a real time domestic violence reporting bracelet.
This roll out was made possible with support from the United States Agency for International Development (USAID) under the PARTNERSHIPS FOR ENHANCED ENGAGEMENT IN RESEARCH (PEER) program and the National Academies of Sciences.
Dr. Juliet Kiguli, the Principal Investigator from Makerere University, along with Dr. Roy Mayega, Deputy Chief of Party at RAN, and Dr. Agnes Nyabigambo, the study coordinator, initiated the PEER program to identify entry points for testing SafeBangle Technologies (a social enterprise based at Resilient Africa Network (RAN) with a mission to create a safer and more secure environment for women and children through innovative, affordable, and creative technology solutions to curb GBV in Africa.) wearable safety bracelet in the informal settlements. This decision stemmed from findings of increased intimate partner violence (IPV) and gender-based violence (GBV) in three informal settlements in Kampala, Uganda, following a longitudinal study, geospatial mapping, and interviews. The project, titled ‘The Impact of the COVID-19 Pandemic on Gender-Based Violence among Women and Girls in Informal Settlements in Kampala,’ highlighted the urgent need for affordable and immediate reporting mechanisms for violence.”
‘’While carrying out a study after the Covid-19 Pandemic, we identified gaps when it comes to reporting and response to Gender Based Violence (GBV) among women in informal settlements. Therefore, we used incorporated the SafeBangle intervention to solve the problem of lack of affordable and immediate reporting mechanisms for violence using a bracelet that reports violence in real time’’ explained Dr. Kiguli.
Innovation details
According to Saul Kabali and Messach Luminsa, the innovators behind SafeBangle from SafeBangle Technologies, hosted at the Resilient African Network Lab. ‘’The inspiration behind SafeBangle came from a deeply personal place. ‘’We heard countless stories of women who couldn’t call for help during moments of danger. We were deeply affected by the story of Aisha, a young woman in a rural village who was attacked while walking home alone at night. With no way to call for help, she felt helpless and vulnerable. This incident made us realize the critical need for immediate reporting alert tools, accessible to women like Aisha. We knew technology could play a crucial role and this incident awakened a strong desire in us to create a solution’’

“While developing SafeBangle, we tested with the users in both rural and urban contexts. We piloted the innovation around Kampala with support from Digital Human Righs Lab and Naguru Youth Health Network as well as it in five districts of Karamoja region with support from Save the Children and Response Innovation Lab. Right now it has become handy in Kamapala‘s informal settlements. We envision a future where SafeBangle becomes a standard tool in the fight against GBV, ensuring every woman feels safe and secure as it has the potential to transform how we respond to GBV in Africa” added Kabali.
HOW THE SAFEBANGLE TECHNOLOGY WORKS
The SafeBangle is wearable technology similar to a smartwatch that sends an alarm by SMS to people chosen by a woman herself if she feels threatened.

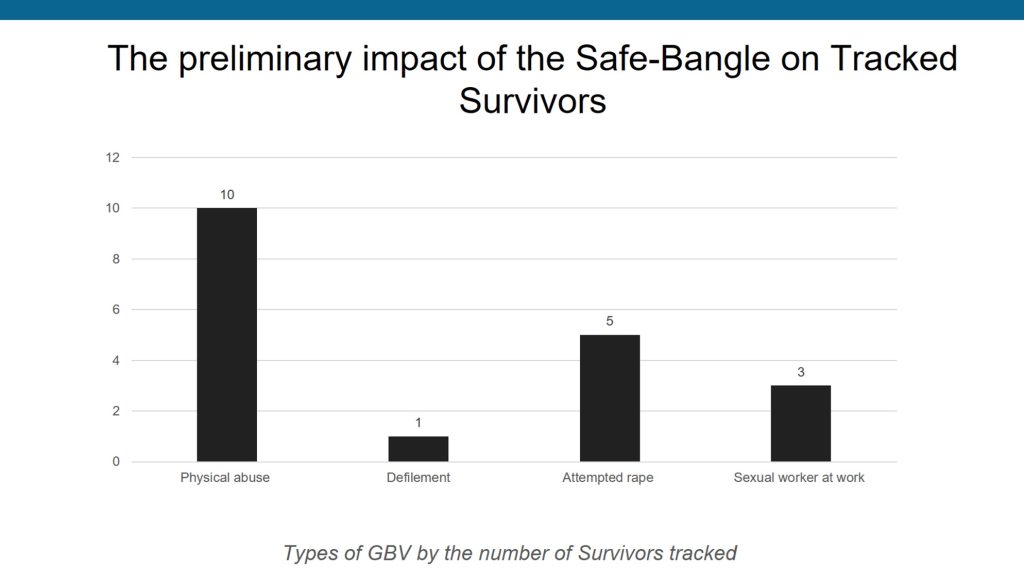
In terms of the acceptability of the SafeBangle innovation as a solution to GBV among at-risk women in informal settlements Of the 72 adolescent girls and women who received the SafeBangle, 22 activated the reporting button, resulting in 19 receiving immediate and appropriate support, including counseling, police intervention, and health services.
All adolescent girls and women who experienced GBV received a phone call from Somero Uganda to discuss the most appropriate intervention, including counseling, police cases being handled by the probation office, referral for health services, and post-exposure prophylaxis. All the GBV survivors received support and are still receiving continuous follow-up.
Researchers conducted a survey among 644 girls and women in Kinawataka (Nakawa Division) and Bwaise (Kawempe Division) to gain insights into awareness and understanding of sexual and gender-based violence among adolescent girls and women in informal settlements. The survey measured socioeconomic factors, mental health symptoms, and exposure to GBV. Focus group interviews were conducted with a separate sample of women over 18 in the settlements to explore responses to GBV.
A tabular representation of the key findings and lessons learned from your study on gender-based violence (GBV)
| Key Findings | Lessons learned |
| Prevalence of GBV. – Overall prevalence: 34.1% of women and girls reported experiencing GBV. – Among adolescents (15-19 years): Over 50% reported experiencing GBV. | – The pandemic highlighted the need for accessible and comprehensive support services for GBV survivors. – Schools emerged as crucial safe spaces for girls, emphasizing their well-being during crises. – Economic independence proved crucial, enabling women to leave abusive environments. – Involving men and boys as allies in GBV prevention efforts is essential. |
| Age-related trends | – GBV prevalence tends to decrease with increasing age. |
| Physical and health consequences. | – Women and girls suffered physical violence, injuries, and deaths, primarily from domestic violence and unsafe abortions due to limited healthcare access. – GBV resulted in unintended pregnancies, unsafe abortions, and increased risk of sexually transmitted diseases (STIs) like HIV/AIDS. |
| Social and economic impact. . | – GBV contributed to family breakups, strained marriages due to financial stress. – Economic hardships forced some women and girls into transactional sex, exposing them to further health risks and exploitation. – Pandemic-related job losses and economic constraints increased financial dependence on abusers, trapping women in violent situations. – School closures and increased household responsibilities limited women’s job opportunities and subjected them to sexual harassment. |
| Psychological effects | – Survivors experienced guilt, shame, anxiety, fear, and suicidal thoughts due to ongoing abuse. |
| Long-term effects | – Post-COVID-19, survivors faced disrupted education, early marriages, pregnancies, social stigma, and persistent mental health issues. |
Reproductive Health Consequences: GBV resulted in unintended pregnancies, unsafe abortions, and increased risk of sexually transmitted diseases (STIs) like HIV/AIDS.
Family Breakdown: The rise in GBV led to family breakups as women fled abusive relationships. Marriages were strained due to increased financial stress.
Transactional Sex for Survival: Desperate for basic needs due to job losses and economic hardship, some women and girls resorted to transactional sex, exposing them to further health risks and exploitation.
One study participant stated, “The time of COVID-19 was so terrible for some of us. We in fact got a lot of diseases from it because you would want to get food and didn’t have money. That way you would be forced to get a man who would use you and pay.” – (FGD_Girls_19–24years_Kinawataka).
Economic Effects: COVID-19 restrictions caused job losses and limited economic opportunities, particularly for women in the informal sector. This increased financial dependence on abusers and trapped women in violent situations.
Limited Access to Employment: School closures and increased household chores limited women’s ability to seek employment, perpetuating gender inequality in the workforce. Some faced sexual harassment from potential employers.
Psychological Effects: Survivors of GBV experienced guilt, shame, anxiety, fear, and even suicidal thoughts due to the constant threat and unpredictability of abuse.
Post-COVID Effects: GBV survivors faced long-term consequences, including disrupted education, early marriage, early pregnancy, social stigma, and persistent mental health issues.
Lessons learned
The pandemic highlighted the need for accessible and comprehensive support services for survivors of GBV, the significance of schools as safe spaces for girls, and the need to prioritize their well-being during crises. Economic empowerment emerged as a significant protective factor for women and girls. Those with greater economic independence were better equipped to leave abusive environments and secure their safety and well-being, while dependent ones suffered abuses. Engaging men and boys as allies in the fight against GBV and involving them in prevention efforts can help promote positive behavior change and foster more equitable relationships.
Recommendations
To address GBV against women and girls, the researchers recommend the following moving forward;
- There is need to integrate technology-driven solutions like SafeBangle into national GBV prevention and response strategies. SafeBangle can be a valuable tool for policymakers as cases of violence that would have gone unreported will be brought to light and the would-be victims will be able to get immediate help from trusted relatives and friends.
- Provide economic opportunities and vocational training for women and girls to enhance their financial independence and reduce vulnerability to violence. There is therefore a need to introduce education and training programs that empower women and girls, by providing them with skills, resources, and opportunities to start their own ventures and to participate fully in community affairs.
- Strengthen and enforce existing laws and policies related to GBV, including laws against domestic violence, child marriage, and sexual assault without discrimination be it for law enforcers, leaders, and employers where such cases were suffocated. Ensure that perpetrators are held accountable through swift and fair legal processes that have no room for corruption.
- Establish and promote effective, accessible, and confidential reporting mechanisms for GBV incidents that provide confidence and can be trusted by survivors to enhance reporting of such incidences of GBV. Community Engagement and Involvement: Involve community leaders, religious leaders, and elders in discussions about GBV to promote gender equality, change social norms, and reinforce the message that violence against women and girls is unacceptable.
- Launch extensive public awareness campaigns to challenge harmful gender norms, report cases of GBV, raise awareness about the consequences of GBV, and promote positive behaviors and attitudes towards women and girls.
- Implement comprehensive sexuality education in schools and communities, educating young people about healthy relationships, consent, and reproductive rights to be able to make informed decisions about their own lives and well-being.
- Engage men and boys as allies in the fight against GBV, encouraging them to challenge harmful masculinity norms and behaviors. This will help minimize GBV because mostly they are the perpetrators. Strengthening Support for Survivors: Provide ongoing support and follow-up services for survivors of GBV mostly counselling services to aid their recovery and facilitate their reintegration into society.
- Provide ongoing support and follow-up services for survivors of GBV, mostly counseling services to aid their recovery and facilitate their reintegration into society.
- Provide avenues to seek free or subsidized services by survivors of GBV medical services and legal processes by survivors of GBV to enhance reporting of GBV cases, access to medical care, counseling, legal support, and other essential services.
- Encourage and support more research and innovations like SafeBangle to curb incidents of GBV.
- A comprehensive and inclusive approach is required. The efforts should involve government institutions, civil society organizations, community leaders, and individuals working together to address the root causes and provide support to survivors.
- Involve media in GBV prevention activities and for enhancing campaigns against GBV mostly on radio and TV.
MORE ABOUT THE STUDY
The core project team, included researchers at Makerere University School of Public Health (MakSPH), Medical College of Wisconsin (MCW) led by Prof. Julia Dickson-Gomez, SafeBangle Technologies, and Somero Uganda, a community-focused NGO, began the project by designing their research protocol and taking a CITI Program course on human subjects social/behavioral research. Team members also met with the Ministry of Gender, Labour, and Social Development (MGLSG) in support of the gender-based violence policy process, Ministry of Health and local government. They also established relationships with the Kampala Capital City Authority (KCCA) and Nakawa and Kawempe probation offices to support legal processes for the GBV survivors. SafeBangle Team also received an award from Defenders Protection Initiative.
You may like
-


Are We Giving Enough Attention to the People Around Us Who Quietly Influence Lives Every Day?
-


The silent teachers: why body donation matters
-


Prof. Isa Kabenge Officially Hands Over Leadership of DABE to Prof. Joshua Wanyama
-


Government Strengthens Public Investment Management Capacity Through Intensive Training at Makerere University
-


Freshers’ Joining Instructions 2026/2027
-


Tribute To Professor Abwoli Yabezi Banana (1951–2026)
Health
The silent teachers: why body donation matters
Published
1 day agoon
June 5, 2026By
Mak Editor
By Assoc. Prof. Erisa Mwaka and Joyce Nabukalu-Kiwanuka
In every hospital, there is a moment when knowledge becomes a matter of life and death. A doctor must know where to place an incision, how to avoid damaging major organs, how to identify a nerve, how to deliver a baby safely, how to interpret a scan, or how to explain disease to a worried family. That knowledge does not begin in the operating theatre, it begins much earlier, in the anatomy laboratory.
For generations, the study of the human body has been the foundation of medical education. The regular use of human bodies for medical training purposes began in the late Middle Ages and spread during the 18th and 19th centuries. Initially, anatomists depended on gallows, poor houses, mental asylums, or jails as sources of bodies. However, the 1960s and 1970s saw the emergence of wilful body donation. Before students become doctors, surgeons, dentists, nurses, physiotherapists, radiographers, and other health professionals, they must first understand the human body in its real form. They must learn not only from books and diagrams, but from the body itself. This is why cadavers, though silent, remain the most important teachers in medical education. In simple terms, a cadaver is a dead human body used by health professions students to study anatomy; and Anatomy is the study of the physical structure and organization of the human body, both at macroscopic and microscopic levels.
As the Department of Anatomy at Makerere University College of Health Sciences prepares to commemorate the “silent teachers” whose bodies are used for medical education on June 11, 2026, Uganda is invited to reflect on a subject that is rarely discussed in the public domain, willed body donation. Body donation simply means a person willfully donates their body for educational purposes after death, and consent to it in life. This is a sensitive topic, but it is also a deeply human one. It touches our beliefs, families, culture, understanding of death, and responsibility to future generations.This commemoration ceremony is not symbolic but, it is a public statement that the contribution of silent teachers is sacred, educational, and deeply appreciated.
To donate one’s body after death is not an ordinary decision; it is an altruistic act of extraordinary generosity. It is a final gift to society. It allows health professions students to learn and appreciate the human body before they treat living patients. Cadavers are therefore not “specimens”, they are silent teachers and partners in medical education who continue to serve humanity even after death. Learning anatomy using a cadaver helps students to understand and appreciate the complexity of the human body, appreciate its natural variations, and develop the confidence and competence needed to serve the public. Students are also taught laboratory etiquette that emphasises dignity, empathy, and utmost respect for the cadavers, which attributes they carry into the clinical years when they interface with hospital patients.
In Uganda, where the demand for health workers continues to grow, medical education must be strengthened at every level. Our country needs well-trained doctors and health professionals who can serve in hospitals, health centres, universities, research institutions, and communities. But good training requires good teaching resources. One of these resources are the silent teachers who never complain, but impart immeasurable knowledge to future health professionals. Modern technology has introduced many useful tools into medical education. Students can now learn from videos, computer applications, digital images, plastic models, three-dimensional models, and virtual platforms. These tools are important and should be embraced, however, they cannot completely replace learning from the real human body. A cadaver teaches what a diagram cannot fully show; the true position of organs, the texture of tissues, the relationship between structures, and the natural differences that exist from one person to another. More importantly, cadaver-based learning teaches respect. It reminds students that medicine is not simply a technical profession, it is a calling rooted in human dignity. The first lesson students learn in the anatomy laboratory is that the body before them belonged to a person who had a name, a family, a story, and a life. That lesson shapes how they later treat patients.
Currently, most, if not all universities in Uganda, and similar settings in Africa use unclaimed bodies for learning Anatomy. The use of cadavers in Uganda is governed by the Penal Code (Anatomy Rules) of 1957 that permits public hospitals to transfer bodies unclaimed for at least 14 days to a medical training institution like Makerere University. Unfortunately, these cadavers are used without the consent of the deceased because most of them are unknown and with no known relatives to claim them. Many opponents to the use of unclaimed bodies opine that the practice is unethical. There is a global push toward ethical use of cadavers in medical education, where a person consents and bequeathes his/her body for medical education when still alive. For this practice to be sustainable, there is a need for a well regulated body donation program. Unfortunately, the concept of willful body donation is still not well understood by many people, and neither has it been a topic of public debate. Further, there are lots of myths surrounding death and dying in Africa, including Uganda that have hindered the establishment of successful body donation programs. Willingness to donate bodies for medical education is however, influenced by several factors including cultural and religious beliefs, respect for the dead and the need to fulfil burial rites, fear for mutilation and disrespect, to mention a few. These concerns are real and should not be dismissed. But they should be addressed with accurate information, openness, and utmost respect.
It is important to understand that body donation does not mean that a person is forgotten. On the contrary, it creates a legacy. A body donor may teach hundreds of future health professionals, in that way, one person’s final act of generosity can touch and save countless lives. This is kind of patriotism is largely unkown in Uganda and we do not speak about enough. We often talk about serving our country through leadership, business, farming, teaching, parenting, or community service. But there is also service beyond life. Body donation is one way of saying: “Even when I am gone, let me contribute to the health of my people.”
Currently, Uganda now has more than 15 universities training medical students and the demand for cadavers for learning anatomy is on the rise. Actually, the supply of cadavers cannot fulfil the demand, and medical educationists need to find alternative source of cadavers. Wilful body donation is the answer.
Uganda needs a national conversation on body donation. There is a need for deliberative public engagement involving various stakeholder including the public, religious and cultural leaders, civic leaders, the media, educationists, health professionals, medical training institutions, etc.
This commemoration ceremony will involve inter-denominational prayers for the silent teachers, and a reflection of their contribution to healthcare in Uganda. We hope this ceremony will provoke public debate on a subject that is hitherto considered a taboo by many. We talked about some of these issues last year, in the first ever such ceremony in Uganda, and have received several requests for more information on the procedure for donating one’s body for teaching purposes upon death. Like President Obama’s said, “yes we can”, an the dialogue starts from you and me. You are all invited for the commemoration ceremony at 9.00 am on June 11, 2026, at the Makerere University School of Public Health auditorium on main campus.
To donate one’s body is to give a final lesson, a final service, and a lasting gift to the nation.
Health
Makerere Health Services Guidance on Ebola Virus Disease (EVD)
Published
5 days agoon
June 1, 2026By
Mak Editor
The Democratic Republic of Congo (DRC) and Uganda recently reported an outbreak of Ebola Virus Disease (EVD), which is a serious and often deadly disease caused by a person being infected by the Ebola virus.
The virus spreads through direct contact with body fluids such as blood, saliva, faeces, vomit, urine, sweat or genital fluids from a person who is infected with EVD.
The symptoms of EVD usually develop after 8 – 10 days from contact with an infected person and may include fatigue, high fever, headache, sore throat, muscle and joint pains, vomiting and diarrhea and in severe cases, bleeding.
What should we do as the Makerere University community?
The Chief, Makerere Health Services, Prof. J.K. Byamugisha advises as follows:
- Avoid unnecessary contact such as shaking hands, hugging etc.
- Place alcohol disinfectants or hand washing equipment at all entry points within the University and ensure everyone is using them.
- Students should sit in single-person chairs while in class, avoiding contact with their neighbours.
- Do not sit too close to one another especially in frequently crowded places such as classrooms, library or any other waiting area.
- While at the University Hospital, wash hands a the gate, use alcohol disinfectant at the reception.
- All patients should have a maximum of one caretaker – others can check on them by calling.
- Avoid bringing luggage to the University Hospital.
- Target to do as instructed by the health worker.
- For further information and guidance on Ebola, please call Dr. Charles Basigara on Tel: 0702 966652 and Sr. Eunice Namubiru on Tel: 0779 950978 (Contact persons for the University Health Services)
Additionally, always look out for and ensure full compliance with Ministry of Health (MoH) Infection Prevention and Control measures such as the one below.


Please find attached detailed communications from Prof. Byamugisha and
the Permanent Secretary Ministry of Health.
Health
Call for Applications: Masters Support in Self-Management Intervention for Reducing Epilepsy Burden
Published
2 weeks agoon
May 25, 2026By
Mak Editor
The Makerere University College of Health Sciences and Case Western Reserve University, partnering with Mbarara University of Science and Technology, are implementing a five-year project titled “Self-management Intervention for Reducing Epilepsy Burden Among Adult Ugandans with Epilepsy.”
The program is funded by the National Institute of Health (NIH) and the National Institute of Neurological Disorders and Stroke (NINDS). One aspect of the program is to provide advanced degree training to qualified candidates interested in pursuing clinical and research careers in Epilepsy. We aim to grow epilepsy research capacity, including self-management approaches, in SSA.
The Project is soliciting applications for Master’s Research thesis support focusing on epilepsy-related research at Makerere University and Mbarara University, cohort 3, 2026/2027.
Selection criteria
- Should be a Master’s student of the following courses: MMED in Internal Medicine, Paediatrics, Surgery and Neurosurgery, Psychiatry, Family Medicine, Public Health, Master of Health Services Research, MSc. Clinical Epidemiology and Biostatistics, Nursing, or a Master’s in the Basic Sciences (Physiology, Anatomy, Biochemistry, or any other related field).
- Should have completed at least one year of their Master’s training in the courses listed above.
- Demonstrated interest in Epilepsy and Neurological diseases, care and prevention, and commitment to develop and maintain a productive career, and devoted to Epilepsy, Clinical Practice, and Prevention.
Research Programs:
The following are the broad Epilepsy research priority areas (THEMES), and applicants are encouraged to develop research concepts in the areas of: Applicants are not limited to these themes; they can propose other areas.
- The epidemiology of Epilepsy and associated risk factors.
- Determining the factors affecting the quality of life, risk factors, and outcomes (mortality, morbidity) for Epilepsy, epilepsy genetics, and preventive measures among adults.
- Epilepsy in childhood and its associated factors, preventative measures etc.
- Epilepsy epidemiology and other Epilepsy related topics.
- Epilepsy interventions and rehabilitation
In addition to a formal master’s program, trainees will receive training in bio-ethics, Good Clinical Practice, behavioral sciences research, data and statistical analysis, and research management.
The review criteria for applicants will be as follows:
· Relevance to program objectives
- Quality of research and research project approach
- Feasibility of study
- Mentors and mentoring plan; in your mentoring plan, please include who the mentors are, what training they will provide, and how often they propose to meet with the candidate.
- Ethics and human subjects’ protection.
Application Process
Applicants should submit an application letter accompanied by a detailed curriculum vitae, two recommendation letters from Professional referees or mentors, and a 2-page concept or an approved full proposal describing your project and addressing Self-Management Intervention for Reducing Epilepsy Burden Among Adults or an epilepsy-related problem.
For more information, inquiries, and additional advice on developing concepts, don’t hesitate to get in touch with the following:
Makerere University College of Health Sciences
Prof. Mark Kaddumukasa: kaddumark@yahoo.co.uk
Mbarara University
Ms. Josephine N Najjuma: najjumajosephine@yahoo.co.uk
Only short-listed candidates will be contacted for Interviews.
A soft copy should be submitted to the Administrator of the Epilepsy Project. Email: smireb2@gmail.com; Closing date for the Receipt of applications is 5th July 2026.
Trending
-

 General2 weeks ago
General2 weeks agoApplications for Admission to Undergraduate Programmes 2026/27
-

 Agriculture & Environment5 days ago
Agriculture & Environment5 days agoTribute To Professor Abwoli Yabezi Banana (1951–2026)
-

 General5 days ago
General5 days agoSylas Ruhweza: A Brief Life Marked by Meaningful Accomplishments
-

 Health2 weeks ago
Health2 weeks agoCall for Applications: Masters Support in Self-Management Intervention for Reducing Epilepsy Burden
-

 General2 days ago
General2 days agoFreshers’ Joining Instructions 2026/2027
