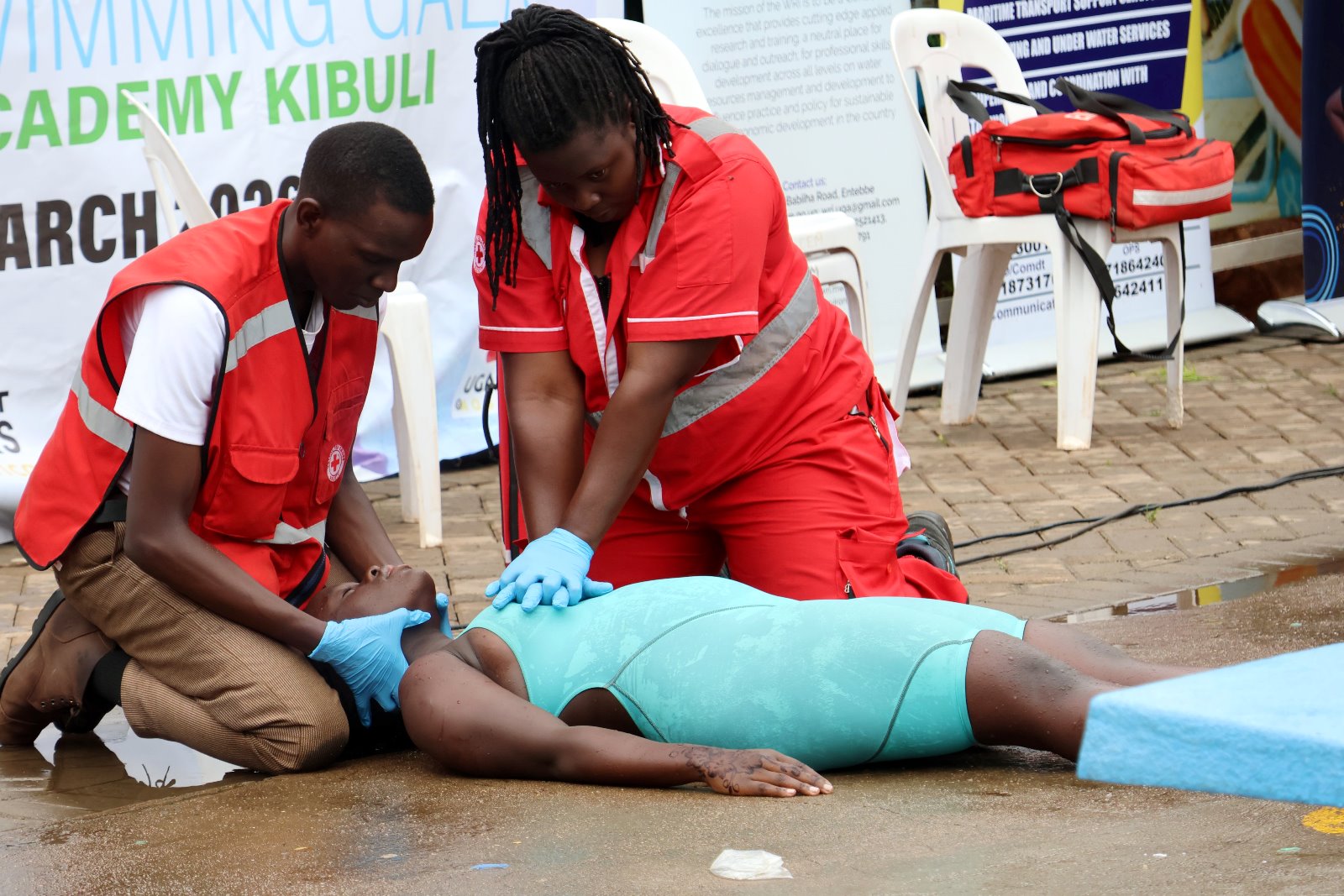
Makerere University School of Public Health, through its Centre for the Prevention of Trauma, Injury and Disability, contributed to the Global Status Report on Drowning Prevention 2024, the first comprehensive global assessment of drowning burden, risk factors, and country-level responses.
Published by the World Health Organisation, the report estimates that approximately 300,000 people died from drowning in 2021, with the highest burden in low- and middle-income countries, which account for 92% of deaths. The African Region records the highest mortality rate, underscoring the urgency of targeted interventions. Children and young people remain the most affected, with drowning ranking among the leading causes of death for those under 15 years.
While global drowning rates have declined by 38% since 2000, progress remains uneven and insufficient to meet broader development targets. The report highlights critical gaps in national responses, including limited multisectoral coordination, weak policy and legislative frameworks, and inadequate integration of key preventive measures such as swimming and water safety education.
It further identifies persistent data limitations, with many countries lacking detailed information on where and how drowning occurs, constraining the design of targeted interventions. At the same time, the report notes progress in selected areas, including early warning systems and community-based disaster risk management.
MakSPH’s contribution to this global evidence base reflects its role in advancing research, strengthening data systems, and supporting context-specific approaches to injury prevention. Through its Centre, the School continues to inform policy and practice, contributing to efforts to reduce drowning risks and improve population health outcomes in Uganda and similar settings.
The full report can be accessed below:
View on MakSPH


 General5 days ago
General5 days ago
 General2 weeks ago
General2 weeks ago
 General2 weeks ago
General2 weeks ago
 General4 days ago
General4 days ago
 General2 weeks ago
General2 weeks ago