Health
Digital Payments Boost Vaccination Campaign Efficiency in Uganda
Published
6 months agoon

KAMPALA, Uganda —Supporting districts to adopt digital payments can significantly improve the efficiency of mass vaccination campaigns in Uganda, even if the gains do not directly translate into higher worker motivation, a new study by Makerere University School of Public Health (MakSPH) researchers has found.
Published on September 10, 2025, in BMJ Global Health, the study examined how helping districts in Uganda transition from cash-based to electronic payments affected vaccination campaign workers. Conducted in early 2023, some four months after the nationwide oral poliovirus vaccination campaign of November 2022, the research assessed the impact of digitised payments on efficiency, timeliness, and worker satisfaction.
With generous support from the Bill & Melinda Gates Foundation, the study was led by MakSPH researchers Peter Waiswa, Juliet Aweko, Maggie Ssekitto Ashaba, Elizabeth Ekirapa-Kiracho, and Charles Opio, in collaboration with Margaret McConnell of the Harvard T.H. Chan School of Public Health, Daniel Donald Mukuye from Uganda’s Ministry of Health, and Andrew Bakainaga from the World Health Organisation (WHO)–Uganda Country Office.
The study’s Principal Investigator and lead author, Assoc. Prof. Peter Waiswa, a health systems researcher at Makerere University School of Public Health, said while the research was conducted in Uganda, its implications are global. He pointed out that some African countries, such as Côte d’Ivoire, Zambia, Tanzania, and Kenya, are already ahead in adopting digital payment systems, while others still lag behind. The study’s findings, he said, are relevant across these contexts and have already informed the work of global actors such as Gavi, WHO, and the Global Fund, who are now integrating digital payments into their own processes.
“This paper is part of several studies we are conducting, but perhaps the most significant,” said Dr. Waiswa, clearly enthusiastic about the findings. “Another outlines the research agenda for digital payments, emphasising the need for more evidence on whether they improve the quality of immunisation campaigns, ensure timeliness and efficiency, and identify which groups face barriers to their use.”

The study was coordinated by MakSPH in collaboration with a network of partners. In Uganda, these included the Ministry of Finance, the Ministry of Health, the World Health Organisation, several implementing organisations, district authorities, as well as telecommunication companies. Importantly, the involvement of Airtel as a non-traditional actor in the study demonstrated the critical role of private sector engagement, often absent in such collaborations, in generating evidence and advancing digital health solutions, particularly in addressing challenges such as timely payments for health campaign workers.
The November 2022 polio campaign, led by the government of Uganda with support from the U.S. CDC and WHO, targeted 8.7 million children under five with the novel oral polio vaccine (nOPV2). Nearly 72,000 teams, including health workers, Village Health Teams, and Local Council representatives, were mobilised nationwide, administering about 10 million doses despite the temporary exclusion of five districts due to the Ebola outbreak at the time.
Building on the campaign, the researchers conducted an exploratory cluster-randomised trial using a mixed-methods approach across 54 districts in Uganda, where they enrolled 2,665 healthcare workers. Intervention districts were trained to use Uganda’s e-cash platform, a government innovation managed by the Ministry of Finance. Introduced in 2017 and formalised in 2019, the cashless system was designed to digitise urgent government payments, enhance efficiency, and improve transparency. It now complements the Integrated Financial Management System, which, though effective for routine payments, was seen as too slow for time-sensitive transactions, including paying campaign health workers, where timely remuneration is critical for maintaining workforce readiness, sustaining campaign momentum, and promptly addressing public health challenges in the communities served.
Intervention studies usually introduce a treatment or program to a group to observe its effects, and the results are compared with a group that does not receive it. The training during the study addressed the delays, leakages, and administrative bottlenecks common in cash-based systems. Intervention districts received instruction on navigating the government e-cash platform, managing user roles, uploading beneficiary data, and generating payment reports, while control districts maintained standard cash payment procedures, serving as a baseline.
Dr. Juliet Aweko, co-author and Research Associate at MakSPH, said the study was timely, observing that health workers are central to successful vaccination campaigns and delayed payments can demotivate them and compromise campaign effectiveness.
“To make digital payments truly work, campaigns must be planned with the workforce in mind. Government and partners need to ensure funds are disbursed on time, streamline and automate registration and verification, and keep accurate records of health workers and their performance. Making mobile money systems compatible and giving workers real-time updates on their payments would not only build trust but also keep them motivated, ultimately improving turnout and ensuring smoother service delivery,” Dr. Aweko stated.

The study found that electronic cash adoption was significantly higher in intervention districts, where 57.5% of workers were paid digitally compared to 44.1% in control districts. What’s more, digital payments did not delay disbursement, as 97.6% of all workers received payment after campaign completion, regardless of method. Still, workers paid via e-cash consistently described the cashless system as convenient, transparent, and cost-effective, citing reduced travel time, lower personal costs, and fewer security risks.
Today, Uganda’s rapidly expanding digital ecosystem provides ground for scaling up cashless payment systems. The Uganda Communications Commission reports that the country has over 43 million active mobile subscriptions, nearly 88% of the estimated 49 million population. Its latest market report shows 26.1 million active internet users, while mobile money continues to dominate financial transactions with more than 33 million accounts and transaction values growing by over 25% annually, according to reports by the Bank of Uganda as of March 2025. This trend reflects a population increasingly reliant on digital platforms, creating a strong opportunity to embed e-payment systems in health service delivery.

For MakSPH researchers Dr. Waiswa and Dr. Aweko, the study evidence confirms that digital payments are both feasible and practical for strengthening the delivery of mass campaigns in low- and middle-income countries like Uganda. With relatively modest support, districts can adopt e-cash systems, providing a scalable model for the health sector. This approach, they suggest, would streamline compensation, reduce administrative delays, and provide a stronger basis for integrating digital payments into future immunisation drives and other public health interventions in the country, thereby strengthening our health systems.
The researchers further emphasised that digitising campaign payments reduces transaction costs and minimises leakages, enabling more funds to reach frontline workers quickly. E-cash also simplifies logistics, strengthens accountability, and enhances financial tracking in health campaigns. These advantages, they found, directly align with the global effort to advance digital transformation in health systems and ensure reliable, transparent worker compensation. The implications also extend beyond just polio, as Uganda continues to rely on mass campaigns for routine immunisation and other outbreak responses, such as measles and yellow fever, where digital payments could improve the efficiency of scarce health resources.
Still, the study acknowledged barriers that could hinder full adoption of a cashless system. Some districts lacked the technical capacity to operate the government’s e-cash platform, upload beneficiary data, and manage user roles. Connectivity issues, limited digital literacy among staff, and occasional system downtimes further disrupted implementation. Additionally, many campaign workers lacked national identity cards or mobile money accounts, making them ineligible for digital payments. To address these challenges, the researchers, among others, recommend targeted capacity building for district finance and health teams, expanded identity and mobile registration for campaign workers, improved internet connectivity, and integration of e-payment systems into routine health planning.
You may like
-


Mak Study Reveals Key Factors Undermining Performance in Biology
-


Harriet Aber’s Research Uncovers Uganda’s Hidden Crisis of Child Substance Use
-


A Night of Memory, Medicine, and Makerere Pride
-


Where Garimoi Orach Built the Field, Komakech Studied Its Exit: Advancing Health Systems Resilience Amid Refugee Arrivals & Repatriation
-


Makerere Graduation Underscores Investment in Africa’s Public Health Capacity
-


Three MakSPH Faculty Honoured with Makerere University Research Excellence Awards 2026
Health
Harriet Aber’s Research Uncovers Uganda’s Hidden Crisis of Child Substance Use
Published
2 weeks agoon
March 18, 2026
In Uganda, children arrive at health facilities every day with fever, cough, injuries or routine illnesses. What health workers rarely recognise is that some of these children are already living with alcohol or other substance use disorders, conditions that complicate diagnosis, delay treatment, and quietly undermine children’s health, development, and long-term wellbeing.
This hidden reality was uncovered by Dr. Harriet Aber Odonga during her doctoral research at Makerere University School of Public Health (MakSPH). Her PhD study, titled “Substance Use among Children in Mbale, Uganda: Health System Landscape and Support Structures,” examined how Uganda’s health system detects and responds to substance use among children aged six to 17 years.
The findings revealed a problem far more widespread than many health workers and caregivers assumed. Nearly one in four children attending health facilities showed signs of alcohol or other substance use problems, with alcohol the most common substance. In the study, a child was classified as having a “probable” substance use disorder when responses to a standard screening questionnaire indicated harmful or dependent patterns of use requiring further clinical assessment.

The discovery adds urgency to an already serious public health challenge. Globally, alcohol and other substance use is responsible for one in five deaths and contributes to more than 200 disease and injury conditions, according to WHO. Across Africa, alcohol alone accounts for 6.4 per cent of all deaths and 4.7 per cent of disability-adjusted life years. In Uganda, alcohol use disorder affects roughly 7.1 per cent of the population and contributes to about 7% of all deaths, while research among young people shows that alcohol exposure often begins early in life.
Despite these risks, most policy and research attention has historically focused on adults and older adolescents. Much less is known about children who begin experimenting with alcohol and other substances earlier in their childhood, a gap Aber set out to examine by studying how Uganda’s health system identifies and responds to substance use among children.
A research question begins
Aber’s interest in the subject began unexpectedly. “I remember seeing a notice calling for PhD students to research child alcohol use,” Dr. Aber recounted. “The phrase struck me immediately. I could not believe that children were drinking alcohol. That moment sparked my curiosity, so I began reviewing the literature on the subject in Uganda. During that search, I came across a study documenting alcohol use among children as young as five years old. That finding was deeply unsettling and raised many questions for me.”
With a longstanding interest in child health, Aber saw the research as an opportunity to investigate a problem that had received little systematic attention. What began as disbelief developed into a doctoral investigation examining how Uganda’s health system identifies and responds to substance use among children. She began her doctoral studies in 2021 at MakSPH under the supervision of Dr. Juliet N. Babirye, Prof. Fred Nuwaha, and Prof. Ingunn Marie S. Engebretsen from the University of Bergen, Norway. She defended her thesis on October 25, 2025, before graduating during Makerere University’s 76th graduation ceremony on February 25, 2026.

Investigating the health system response
Aber’s study examined four key questions. It measured how common substance use disorders are among children visiting health facilities. It assessed whether health facilities are equipped to screen and manage these cases. It evaluated whether screening tools are acceptable to children, caregivers, and health workers. It also examined how families seek help when children begin using substances.
To answer these questions, the research used a mixed-methods design combining quantitative surveys and qualitative interviews. Aber collected data from 834 children attending health facilities in Mbale District, assessed 54 health facilities in the district to determine their readiness to screen and manage substance use disorders, and interviewed health workers, caregivers, and children to understand experiences of care and barriers to seeking help. Additional surveys involving 602 children and 355 caregivers examined help-seeking patterns and support structures.
Quantitative data were analysed to estimate prevalence and identify associated risk factors, while qualitative interviews provided insight into how families, communities and health workers respond when children begin using substances.
What the research found

Data collected between 2023 and 2024 across health facilities in Mbale District in Eastern Uganda showed that substance use among children was far more common than many health workers and caregivers assumed. Alcohol use disorder emerged as the most prevalent form of substance use disorder among children in the study. The analysis also showed that children were significantly more likely to use substances if they were exposed to peer or sibling use, lived in lower-income households, or experienced strained relationships with caregivers.
The research also revealed major health system gaps. Only 19 of the 54 health facilities assessed, representing 35 per cent, met the minimum readiness criteria required to screen, diagnose or manage substance use disorders. Many facilities lacked trained staff, standardised screening guidelines, and clear referral pathways for specialised care.
Aber explained that substance use often goes undetected because it is rarely the primary reason children visit health facilities. “Substance use is hidden,” she asserted, reflecting on evidence from her doctoral study. “While health workers are treating other illnesses, some children coming to these facilities are already struggling with alcohol or other substances.”
She added that early substance use can have lasting consequences for children’s development. “Risk was higher among children exposed to peer or sibling substance use, lower household income, lower caregiver education, and strained child-caregiver relationships. The public should be concerned because early substance use affects brain development, mental health, education completion, and long-term well-being.”
Families often navigate the problem alone

Her research also examined how families and communities respond when children begin using substances. She found formal help-seeking to be rare. Many caregivers relied on informal networks, including relatives, teachers, religious leaders, and local authorities. Health services were seldom the first point of support.
Meanwhile, punitive responses such as discipline or punishment were sometimes used by caregivers attempting to stop the behaviour of substance use among children, but these responses rarely addressed the broader social and family pressures influencing the vice.

One encouraging finding emerged from her study’s assessment of early detection tools. Aber evaluated the use of the CRAFFT screening tool, a short set of structured questions used by health workers to identify whether a child may be using alcohol or other substances. Children, caregivers, and health workers generally found the questions from the tool easy to understand and acceptable to use. In the study, over 85 per cent of children reported the questions were easy to answer, and nearly nine in ten caregivers were comfortable with the screening process.
These findings, however, suggest that routine early detection could be integrated into primary healthcare within the communities. “If policymakers were to act on one finding from my research, I would prioritise integrating routine, age-appropriate substance use screening into primary healthcare,” Aber argued. “With proper training and referral systems, health workers can identify early risk and support children before the problem escalates.”
Training across nutrition, public health and health systems
Aber’s approach to the problem reflects a research journey shaped by training across multiple areas of child and public health. She first studied Food Science and Technology at Kyambogo University, graduating in 2011, before specialising in Nutrition during her Master of Public Health at Makerere University, graduating in 2015, before embarking on her doctoral training in Public Health at the School, completing in 2025 to graduate at Makerere University 76th Congregation.

Before beginning her PhD, she worked on nutrition research and later coordinated studies examining climate risks, anticipatory humanitarian action and community health systems. This background shaped how she approached substance use among children, not as an isolated behavioural problem but as an issue influenced by broader health and social conditions.
“I do not see child substance use as a problem with a single cause,” she noted. “It is influenced by biological, psychological, social, and system-level factors. My nutrition training helped me appreciate how substance use intersects with broader child health concerns such as mental health, family stress, and even food insecurity.” These pressures are visible in her research site in Mbale, where environmental shocks, economic hardship, and family instability persistently shape daily life. Recurrent landslides and livelihood disruptions place strain on households, and adolescents facing stress or instability may turn to substances as a coping mechanism, she holds.
From evidence to solutions
Completing her PhD has now shifted Aber’s perspective from documenting problems to identifying solutions for social impact. “Completing my PhD shifted my perspective from simply generating evidence to actively providing solutions,” she observed. “Child health challenges such as substance use, nutrition, and climate-related risks are interconnected. As a researcher, I have become more systems-focused, and as an advocate, I feel a stronger responsibility to ensure evidence informs policies that improve children’s wellbeing.”

For Aber, that responsibility extends to the families whose experiences informed the research. Parents, teachers, and health workers often notice behavioural changes first, even when they feel unprepared to respond. Listening without judgment, recognising warning signs, and linking children to appropriate support can make a significant difference, she noted, especially in a context where formal services remain limited.
Her research ultimately sends a clear message for Uganda’s health system. Children affected by substance use are already present in communities and health facilities. Detecting the problem earlier, strengthening screening systems, and equipping frontline health workers with appropriate tools could significantly improve outcomes for vulnerable children.
Behind the research journey stood a wide network of support, including MakSPH supervisors and doctoral committee, the TREAT consortium, the MakSPH PhD forum, the Health Development Centre secretariat, study participants, research assistants, family and friends, and funding support from the Government of Uganda through the Makerere University Research and Innovations Fund (MAKRIF) and the Norwegian Research Council, all of whom she remains grateful.
Aber’s research ultimately points to a critical gap in Uganda’s health system. Children affected by substance use are already present but remain largely invisible. Without routine screening, trained health workers, and clear referral systems, opportunities for early intervention are often missed. Addressing this gap, as indicated by her study, goes beyond clinical care. It requires strengthening how the health system recognises and responds to emerging risks that affect children’s long-term health and development.

By Carol Kasujja and Zaam Ssali
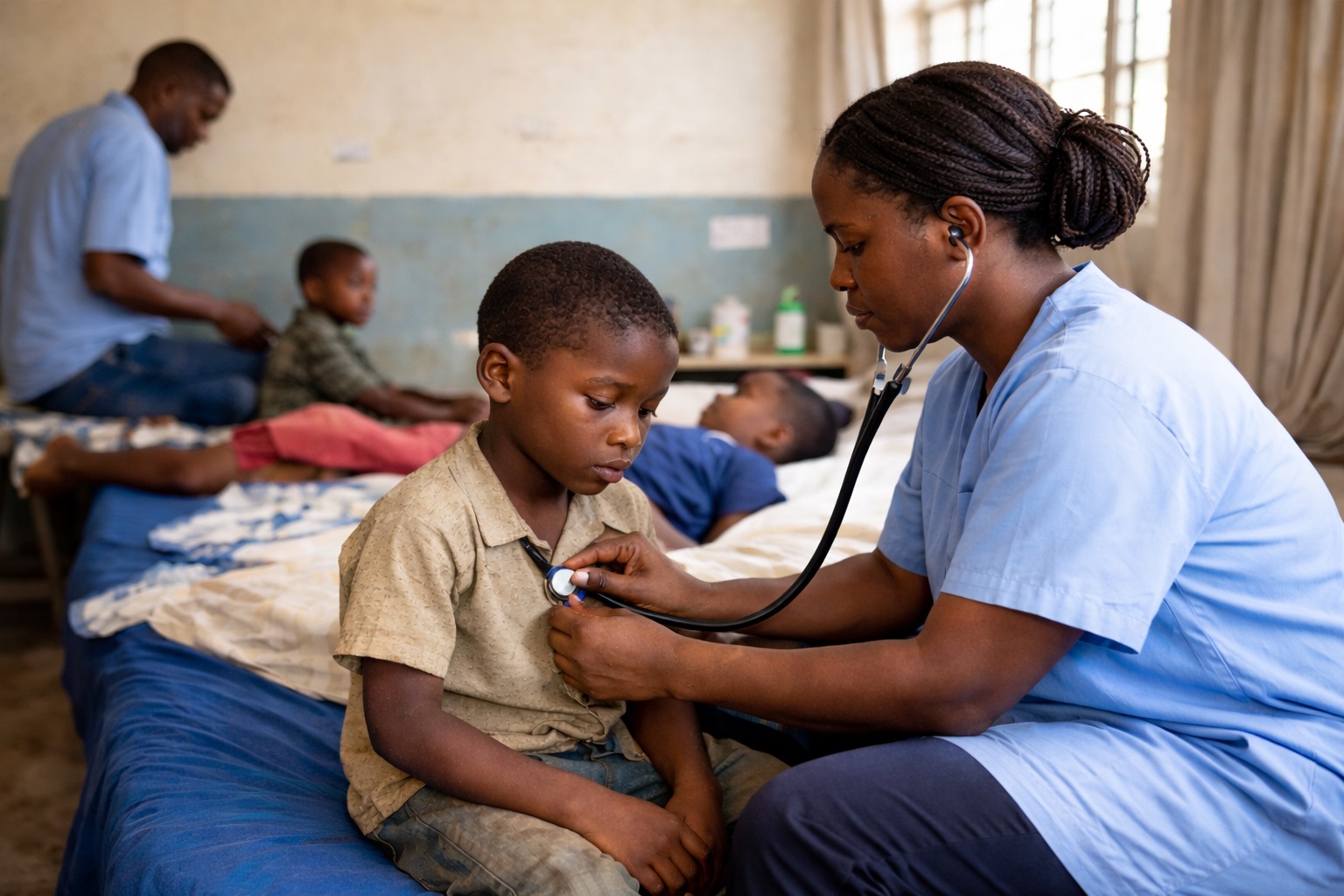
Medical students at Makerere University have been urged to wear the white coat with humility as they begin their journey in the medical profession.
The call was made during the White Coat Ceremony held on Thursday at the Makerere University College of Health Sciences in Mulago.
The White Coat Ceremony marks the beginning of a new journey in healthcare and symbolises professionalism, compassion and excellence. It represents not only the mastery of medical knowledge but also a promise to always place patients at the centre of care. It is a commitment to listen, advocate, heal, and treat every individual with dignity and respect.
“We would have given you a suit, but the symbol of the white coat reminds you that you are here to work. White signifies purity in service. You are in medical school because you are among the best, and you have some of the best lecturers,” said Bruce Kirenga, the Principal of the College of Health Sciences.

Prof Kirenga lauded the students for their dedication to a path dedicated to preserving lives and urged the students to serve with dedication and protect the image of health workers.
“These days, you can use Artificial Intelligence to generate entire coursework, but when it comes to practice, remember the university has an AI policy and you must use it responsibly. In medicine, you take responsibility for your decisions. AI may make life easier, but you must learn and use your hands. Go where the patients are,” he noted.
Prof Kirenga also reminded the students that a medical career offers different paths, including research, teaching, clinical care, and administration.
“As first-year medical students, support each other. Find peers to share your struggles with, especially those in your year. Get mentors and coaches. It took me 26 years to become a Principal, so find mentors who can guide you,” he advised.

Speaking at the event, Sabrina Kitaka, a senior lecturer at the medical school, urged students to uphold the values expected of someone putting on the white coat by being humble and making sure that they connect with their patients.
“Wearing a white coat is a symbol of your commitment to a profession full of honour. This moment is like a rite of passage, from adolescence into adulthood. Joining this noble profession does not make you more important than other students. Be humble,” Dr Kitaka said.
She also encouraged the students to show kindness and compassion to their patients.
Addressing the students, Dr Idro Richard, the Deputy Principal at the College of Health Sciences, called upon the students to always make sure that they keep patients secrets.

“People will come to you and share secrets they have never shared even with their closest family members, do not share people’s pains. If one of you makes a mistake the public will blame all the fraternity so handle your patients with dignity. Always place yourself in the life of those patients when you are in the ward,” Dr Idro, said.
Dr Idro reminded the students to always think of their safety while on the ward by avoiding open shoes.
“Be smart for your own safety, always wear closed shoes, a needle can fall and hurt your legs when you are wearing open shoes. Maintain the excellence you had when you joined and avoid doing life alone,” Dr Idro said.
He further advised the students to always create time and have fun because it is not all about medicine

“Have an open mind, have some fun and also learn other things like soft skills, write, sell and travel. You are in the best School with the best teachers do not allow mediocrity. Avoid cheating, laziness, drugs and betting,” Dr Idro, noted.
In her speech, Anne Atukunda Ronaldine, the chairperson of the Makerere University Medical Students Association (MUMSA), told the first years that they are privileged to join the College as it celebrates a century of excellence.
“Be your brother’s keeper. You will make it together if you work together as a class. Do not avoid your lectures. Medical school is a lot of work, but it gives back,” Atukunda said.

During the ceremony, the College of Health Sciences safeguarding and inclusion champions encouraged students to speak up and report any form of harassment, abuse, or unsafe situations, noting that safeguarding is everyone’s responsibility.
The champions reminded students that creating a safe learning environment requires respect for one another, responsible behavior, and the courage to raise concerns when something is not right. They also urged the new students to support their peers and make use of the available safeguarding channels whenever they feel unsafe or witness misconduct.
The Champions also called upon their peers to support students with disabilities so that no one is left behind. It was a proud moment for many first-year students to finally see themselves wearing white coats, as it was a dream come true for many. The event concluded with a cake-cutting ceremony and a dinner.
Health
82% Stressed: Uncovering the Hidden Mental Health Burden Among Kampala’s Taxi Drivers
Published
3 weeks agoon
March 12, 2026
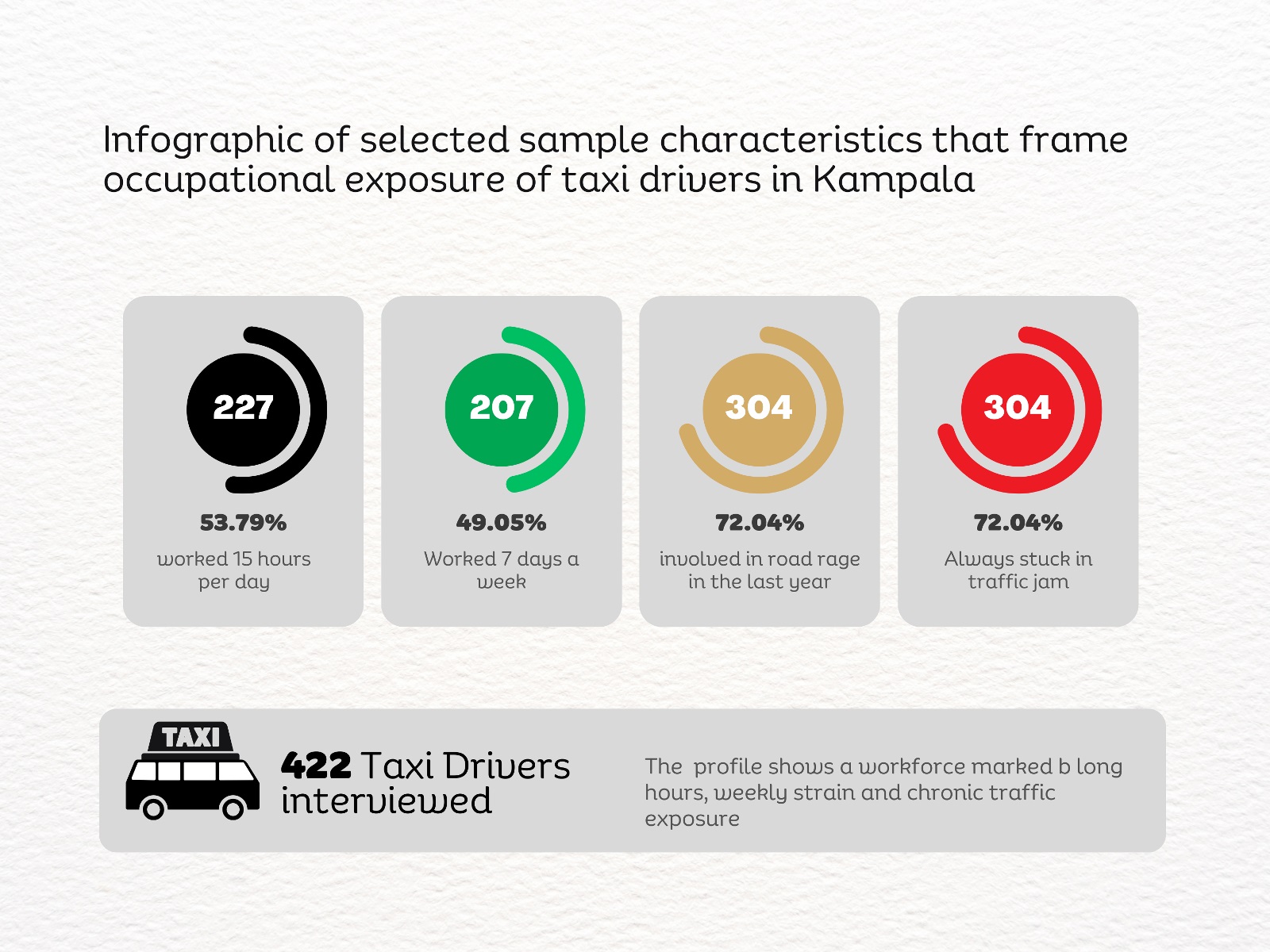
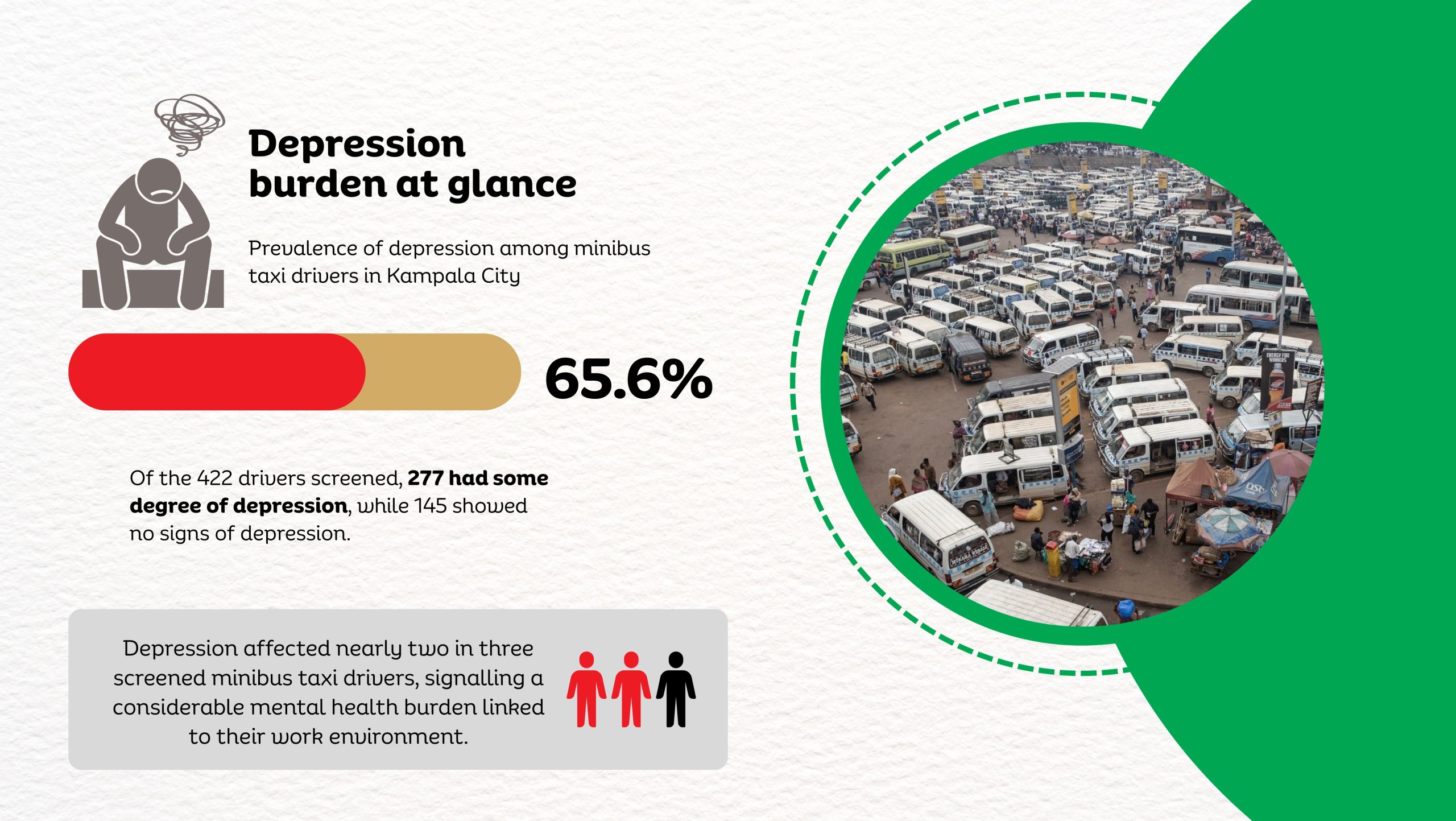
A new study by Dr. Linda Kyomuhendo Jovia, a medical doctor and graduate of the Master of Public Health programme at Makerere University School of Public Health, has found high levels of psychological distress among minibus taxi drivers operating in Kampala’s major taxi parks. In a cross-sectional survey of 422 drivers across Old, New, Kisenyi, Usafi, Namirembe, Nakawa, and Nateete parks, nearly two-thirds screened positive for symptoms of depression (65.6%), while anxiety affected more than 70%, and stress an estimated 82%. The findings point to a largely overlooked occupational health concern within the city’s informal transport sector, where long working hours, economic pressure, poor sleep, and prior road accidents were associated with higher levels of mental strain.
Before sunrise settles over Kampala, Old Taxi Park is already awake. White minibuses marked with the blue stripe of Uganda’s public service taxis sit jammed bumper to bumper, their noses pointed toward narrow exits that will soon release them into the city’s traffic. Dust clings to the windows. Torn seats peek through sliding doors. Diesel hangs low in the air. Conductors slap the metal sides of vans and shout destinations into the morning.
“Kireka! Banda! Bweyogerere!” The calls overlap until they become a steady roar.
Passengers squeeze through narrow corridors between vehicles where there was never meant to be walking space. Hawkers weave through the crowd with trays of roasted maize and boiled eggs. Somewhere, a small radio crackles. Nearby, two conductors argue over whose turn it is to load passengers. This scene is how Kampala wakes, in diesel fumes, shouted destinations, and the quiet urgency of people trying to earn a living before the traffic tightens its grip on the day.
Handwritten route boards fixed to the taxis signal their destinations: Masaka “A” Stage, Kaguta Road, Nakawa, Namirembe, Ntinda, Gayaza, Nansana, and Entebbe, guiding passengers through the organised chaos of the park. Behind every steering wheel sits someone doing the arithmetic of survival. Drivers wake before dawn to secure a place in the queue. For many, sleep is short, interrupted, and rarely restorative. The day stretches across long hours of traffic, uncertain earnings, rent, school fees, and taxi levies, including annual payments of about UGX 720,000. Passengers today mean dinner tonight. Yet inside the noise of the taxi parks, another story has remained largely invisible.
Across Uganda, an estimated 400,000 taxis move millions of passengers every day, forming the backbone of the country’s informal transport system. But almost nothing is known about the psychological toll on the drivers who keep it running.
That gap is what drew Dr. Kyomuhendo into Kampala’s taxi parks. What she uncovered were levels of depression, anxiety, and stress far higher than many had imagined.
A Medical Doctor Turning Toward Public Health
Born on 23 July 1994 to Mr. Muhigwa Lawrence and Ms. Kataito Jacqueline, Dr. Kyomuhendo grew up in Hoima District in western Uganda. Her early education took her from St. Christina Nursery School to Budo Junior School before she continued to Trinity College Nabbingo and later Mount Saint Mary’s College Namagunga for Advanced Level, where she studied Biology, Chemistry, and Mathematics.
In 2014, she earned a government scholarship through the Public Universities Joint Admissions Board and enrolled for a Bachelor of Medicine and Bachelor of Surgery at Busitema University, graduating in 2019.
During her medical internship at Masaka Regional Referral Hospital, she began noticing a troubling pattern in the cases arriving at the wards: road traffic injuries, complications of chronic diseases, severe malaria in children, and obstetric emergencies that might have been prevented with earlier intervention. Many of the crises doctors were treating, she realized, had begun long before patients reached the hospital. “They were symptoms of deeper problems,” she recalls.
Public health offered a way to investigate those underlying causes. In 2022, she enrolled in the Master of Public Health Distance programme at Makerere University School of Public Health, where students are trained to examine health problems not only at the bedside but across entire populations. Guided by Associate Professor Lynn Atuyambe, a respected scholar in Community Health and Behavioural Sciences at MakSPH, and Dr Juliet Kiguli, Senior Lecturer and public health anthropologist, the student’s work benefited from strong academic stewardship.

Uganda’s road transport system is dominated by motorcycles and 14-seater minibus taxis. About 15,000 operate in the Kampala Metropolitan Area alone.
These drivers navigate congested roads, pollution, erratic traffic patterns, and long working hours. Their workday often begins before dawn and stretches deep into the evening.
“They are important in Uganda’s transport industry,” Kyomuhendo said. “Yet they seem to be overlooked in our society.”
While commuting through Kampala during her studies, she began to notice the lives of taxi drivers. Arguments between passengers and conductors were common. When tensions rose, someone would eventually mutter the same question in Luganda.
“Oba abasajja ba takisi baabaki?” loosely to mean, ‘What is wrong with taxi men?’
The question lingered, and in June 2024, social media campaigns marking Men’s Mental Health Awareness Month pushed her to think about the issue differently. What if the behaviour many passengers dismissed as impatience or aggression was linked to something deeper? To her, taxi drivers seemed an unlikely but revealing group to study.
“They carry the responsibility for passengers’ lives every day,” she says. “Yet very little attention is paid to their own well-being.”

For instance, Kampala City Authority (KCCA) documents that between 2019 and 2024, geolocated crash data reveal a dangerous road environment in which Kampala’s taxi drivers operate daily. A total of 1,878 vulnerable road users, including pedestrians, motorcyclists, and cyclists, were killed in crashes involving motor vehicles, with buses and minibuses linked to 281 deaths, most of them pedestrians (147) and motorcycle occupants (131). Fatalities were heavily concentrated along major corridors such as Jinja Road, Kibuye–Natete Road, Bombo Road, and Ggaba Road, while for pedestrians, the most dangerous segments included Gayaza Roundabout (Kalerwe) and Kyebando Police Post along the Northern Bypass and Entebbe Road, where fatality densities reached 27–28 deaths per kilometer. These patterns highlight the high-risk traffic environments in which taxi drivers work, specifically busy arterial roads and bypass intersections where pedestrians, boda bodas, and public transport vehicles compete for space. These conditions contribute to the broader pressures that shape drivers’ safety, well-being, and mental health.
Research in the taxi parks
Her dissertation set out to answer two questions: how common are depression, anxiety, and stress among taxi drivers in Kampala, and what factors contribute to them? The study surveyed 422 male drivers across seven major taxi parks: Old, New, Kisenyi, Usafi, Namirembe, Nakawa, and Nateete, using a multistage sampling approach designed to ensure representation across the city’s transport hubs.
Participants completed structured interviews on socio-demographic, occupational, lifestyle, use of habit-forming substances, medical, and environmental factors. Mental well-being was assessed using the Depression Anxiety Stress Scale (DASS-21), a widely used screening tool in mental health research.
The data were analysed using statistical models that allowed Kyomuhendo to examine how occupational conditions, lifestyle factors, and health status interacted to shape mental well-being.
The study reflected the epidemiological training embedded in MakSPH’s Master of Public Health programmes, where students are encouraged to investigate real-world health challenges through evidence-based research.
Conducting interviews inside the taxi parks meant stepping into one of the most unpredictable environments in the city. “The atmosphere was survival for the fittest,” Kyomuhendo recalls.
Stories behind the statistics
The fieldwork brought moments that stayed with her long after the questionnaires were completed. One driver laughed when asked how he coped with stress. “I don’t drink or smoke,” he said, suggesting that multiple relationships were his way of managing the emotional strain of the job.
The answer was not in the questionnaire, and they both laughed. Yet the moment captured something deeper about life in the taxi parks: humour often hides exhaustion.
Another driver told her he had spent years buying herbal medicine for a hernia that never healed. Every month, he spent close to 100,000 shillings, hoping the treatment would eventually work. She advised him to seek hospital care, a conversation that stayed with her.
“Sometimes people spend far more trying to manage a problem than it would cost to treat it properly,” she explains.
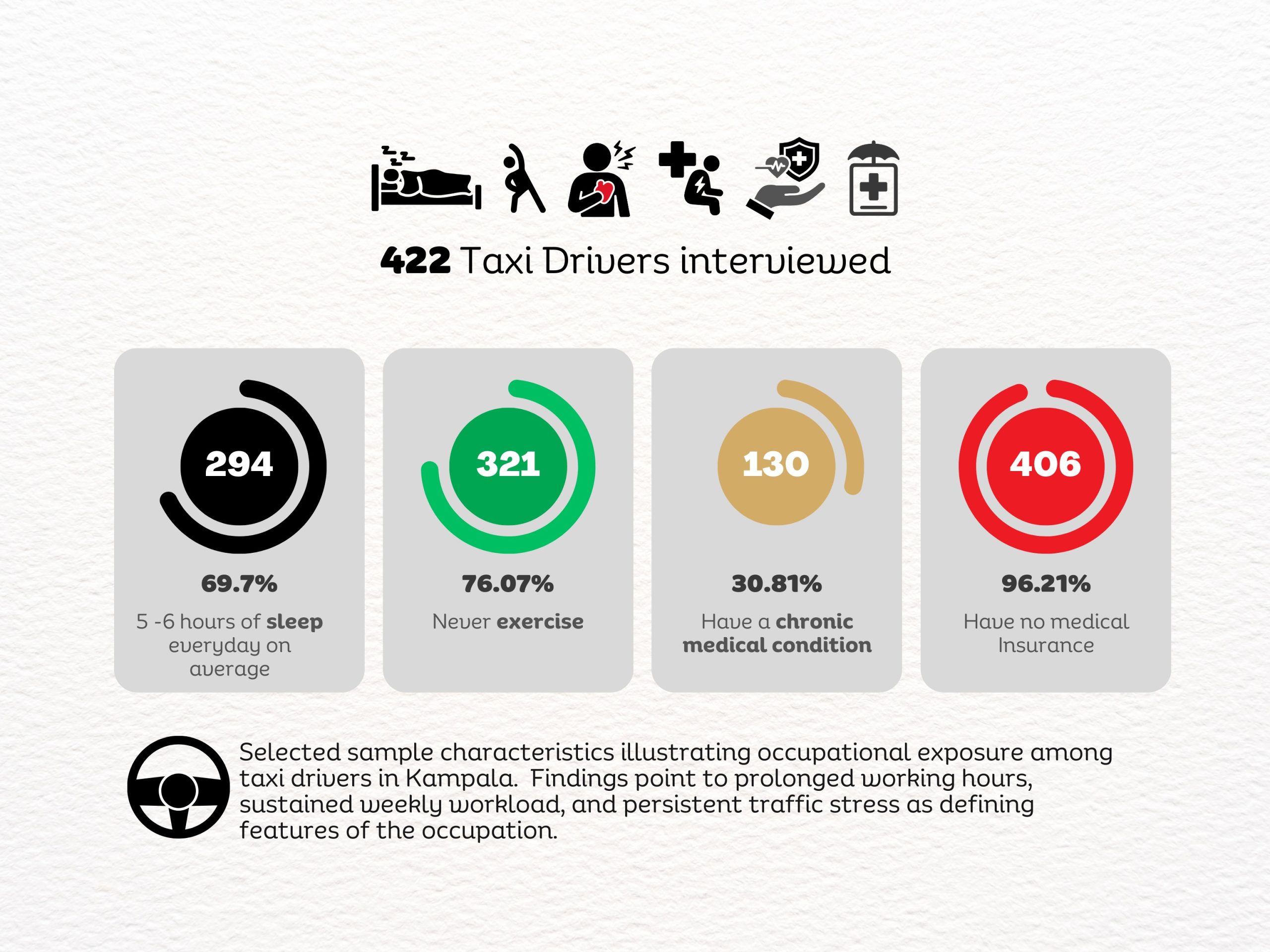
When the data were analysed, nearly two-thirds of the drivers screened positive for symptoms of depression. More than 70 percent had symptoms of anxiety, and over 80 percent reported levels of stress. The psychological burden was far heavier than most people had assumed.
Several factors stood out. Drivers who had experienced road accidents in the previous year were significantly more likely to report depression. Chronic medical conditions and a family history of mental illness also increased the risk.
Sleep deprivation emerged as one of the most important predictors. Drivers who consistently slept fewer than seven hours per night were far more likely to report anxiety and stress. Also, economic security mattered. Drivers who owned their vehicles were substantially less likely to experience anxiety compared to those who rented taxis or paid daily remittance fees to vehicle owners. In other words, psychological distress followed the same lines as economic pressure.
More than a transport problem, and the silence around men’s mental health
The implications extend beyond the drivers themselves, she observed. Mental health affects concentration, reaction time, and decision-making. All abilities that are critical for safe driving in a city known for congestion, unpredictable traffic, and frequent road hazards, including flooding, among others.
“If drivers are anxious or sleep-deprived,” Kyomuhendo explains, “there is a risk they may struggle to follow traffic rules or respond quickly to hazards.”
In a transport system that carries millions of passengers daily, the well-being of drivers becomes a matter of public safety. The findings suggest that mental health among taxi drivers should be treated as both an occupational health issue and a transport policy concern.
During interviews, Kyomuhendo noticed another pattern. Few drivers openly described themselves as depressed or anxious. Instead, stress appeared through jokes, casual references to alcohol or relationships, or long pauses followed by silence.
Men’s mental health remains a difficult subject in many communities. “Men’s mental health is a serious public health issue that should not be ignored,” she says.
Breaking the stigma will require awareness campaigns, stronger occupational protections, and greater attention from both health authorities and transport regulators, she proposes.

A different way of seeing the city?
This research also changed how Kyomuhendo sees Kampala. Where passengers notice congestion or impatience, she now sees the pressures shaping the people behind the wheel. “It made me appreciate the men who show up every day and work hard despite their struggles,” she says.
One driver confided in her about the pressures of the job. “People will not help you unless they know the problems you are facing,” he said.
The city and its drivers
By late afternoon, the taxi parks are as crowded as they were in the morning. Conductors still shout destinations into the traffic. Engines idle in long rows of white vans waiting for passengers. Drivers lean against steering wheels, hoping the next arrival will finally fill the vehicle.
The city keeps moving because they do. Most passengers step into these taxis thinking only about where they are going—work, home, school, or the market. Few stop to consider the pressures carried by the people behind the wheel.
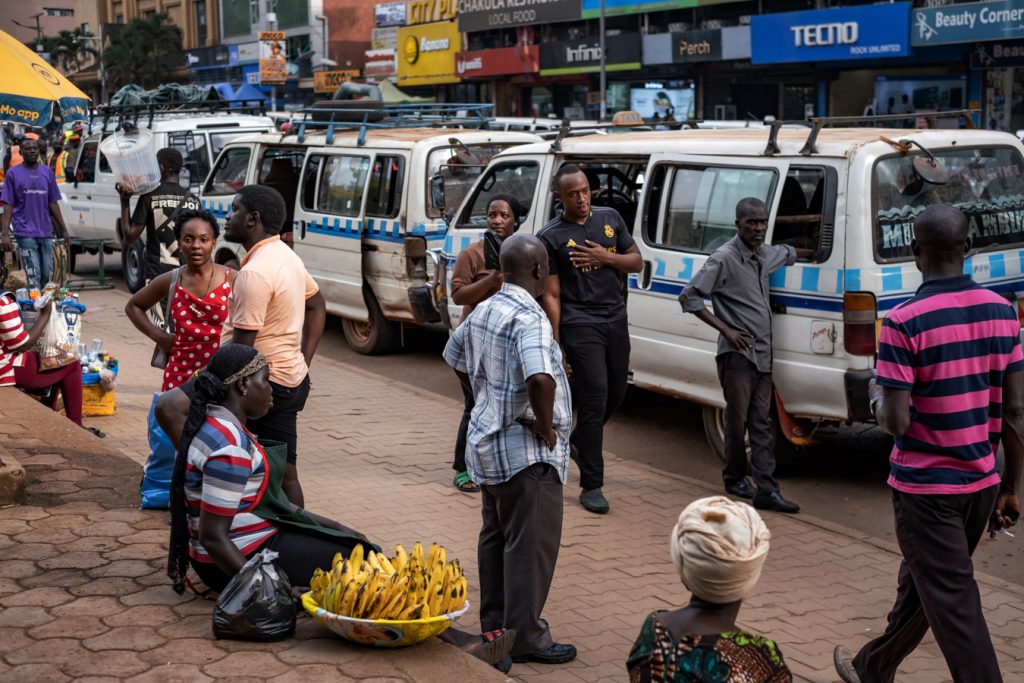
Yet Kyomuhendo’s research suggests that beneath the noise of the taxi parks and those car hoots on the streets lies something far quieter and far less visible: a level of stress, anxiety, and depression that touches not only the drivers themselves but also the safety of the passengers they carry and the communities they serve.
Each morning, the vans will still line up bumper-to-bumper. Conductors will still shout destinations into the traffic. Kampala will still climb inside and move.
If nearly half a million taxis keep Uganda moving every day, who is protecting the minds of the people behind the wheel?
Trending
-

 Law1 week ago
Law1 week agoPre-Entry Examination for Admission to the Bachelor of Laws for 2026/2027 AY
-

 Research2 weeks ago
Research2 weeks agoMakerere Strengthens Research Ethics as Leaders Call for Reforms in Governance, Integrity, and Student Support
-

 General2 weeks ago
General2 weeks agoCall For Applications for Masters Research Support: Drug Safety in Uganda
-

 General2 weeks ago
General2 weeks agoMakerere Hosts Transformative Careers Fair, Bridging Students to the Future of Work
-

 General2 weeks ago
General2 weeks agoCareer Expo 2026 Concludes as Students Gain Industry Insights, Career Guidance, and Networking Opportunities
